Introduction
Trends in use and abuse of drugs in Norway
Treatment principles and facilities
Norwegian personal follow-up studies
Prophylactic measures
Author: Nils RETTERSTÖL
Pages: 27 to 44
Creation Date: 1976/01/01
Norway is the Scandinavian country where drug dependence traditionally has been least widespread. The wave of drug dependence that has swept over Europe has hit the Scandinavian countries hard, amongst them Norway. In the following we shall elucidate how the development has been in this country, as regards both adolescent drug dependence and more traditional dependence on sedative and hypnotic drugs. Particular attention will be paid to the development during the past few years. Then we shall discuss the therapeutic programmes which in time have been worked out and to some extent co-ordinated and integrated on the basis of national planning. Scandinavia in general and Norway in particular have rich traditions as regards clinical psychiatric follow-up studies. This applies especially to psychosis psychiatry. However, this tradition has been extended to include also drug dependence. Comprehensive follow-up studies are available, partly on traditional drug dependents and, of recent date, on adolescent drug dependents. These studies are personal follow-up examinations, in part of hospitalized patients, in part of patients treated in out-patient setting. The follow-up studies - which are still very fresh - have been published in Norwegian only. By way of conclusion, we shall review the prophylactic measures that have been developed against drug abuse. These are extensive and systematized. In Norway there is broad multi-disciplinary and unanimous political agreement concerning preventive measures.
Of international surveys treating some of the topics discussed in this paper may be mentioned the works of Retterstöl [ 22] , [ 23] and of Teigen [ 30] .
Under the auspices of the National Institute for Alcohol Research (Statens institutt for alkoholforskning) a very good job has been done of recording drug habits among Norwegian youth from 1968 up to 1975. This mapping out runs continuously. Using anonymously completed questionnaires, representative population surveys have been made every year since 1968 of young people aged 15 to 20 years, at first only in Oslo, later in other towns too. The basic findings as to trends in use of drugs will be reported below. The first registrations apply to cannabis only, whereas other drugs were also included after a few years.
Studies made in 1968 [ 4] showed that 5.3 per cent of the adolescents in Oslo in the above-mentioned age groups had tried cannabis on one or more occasions. A corresponding study made in 1969 revealed an incidence of 5.1 per cent [ 5] . In 1970, the number of cannabis users had risen to 8 per cent, in 1971 to 15 per cent, in 1972 to 18.7 per cent, figures indicating a fairly steady increase in the use pattern. But in 1973 it looked as if the tide was about to turn in that the rate was then 18.4 per cent [ 13] . In 1974 the percentage was 20 and in 1975, 19 [ 20] , [ 27] . Even if one has to reckon with a certain inaccuracy in studies of this type, the findings suggest that the increase in use of cannabis among young people in Oslo has stagnated during the course of the past five years. Certain trends have appeared in the developmental patterns, however. While the earlier materials showed a heavy preponderance of male adolescents who had experimented with the drugs, the surveys of the last three years reveal an equal number of female adolescent users. A happy feature in the last investigations is that drug use appears to be decreasing in the youngest age groups, a finding which augures well for the future. When evaluating the figures indicated, it should be borne in mind that the majority of those who have tried cannabis reportedly have used it once or only a few times. There are, however, about 10 per cent who admit to having used the drug more than 10 times.
With reference to other drugs, the rates are considerably lower. However, about 4 per cent report that they have tried LSD and about 6 per cent that they have tried amphetamines. There has been an increase of this percentage, but at the moment it seems to have stopped. The corresponding rates for sniffing are fairly constant: 10, 9, and 8 per cent respectively, the lowest rate being that for 1975.
Other towns
Surveys undertaken in other Norwegian towns give certain indications of the drug use pattern among adolescents. A study made in 1970 in the Tønsberg area - a small town in the south-eastern part of Norway - revealed that 6 per cent of the young people had tried cannabis, a surprisingly high rate for a provincial town [ 2] . Yet more astonishing was the finding that amphetamines had been tried by 2.7 per cent of the Tønsberg youth against 1.9 per cent of the Oslo youth during the same year, and that 8.6 per cent of the Tønsberg youth had been engaged in sniffing one or more times as opposed to 6 per cent of their counterparts in Oslo. The 1970 study disclosed the proportion of each sample which had tried at least one of the drugs: marihuana or hashish, LSD, and amphetamine, or who had been involved in sniffing. In Oslo as in Tønsberg the rate proved to be about 12.5 per cent, that is every eighth adolescent. For the majority the consumption had reportedly been modest and was a thing of the past.
Bergen is the second largest city in Norway with a population slightly above 200,000. Since 1971 [ 26] , the drug habits among adolescents in this town have been registered at two-yearly intervals. In 1971, 5.5 per cent admitted to having experimented with cannabis on one or more occasions, a finding corresponding to the rates found in Oslo in 1968 and 1969 and in Tønsberg in 1970. For other drugs, the figures were considerably lower than in the two latter cities. Conversely as many as 9 per cent stated that they had been engaged in sniffing, a rate which seems rather high.
The situation in Bergen has been followed through corresponding surveys in 1973 and in 1975 [ 26] . In 1973, 9.7 per cent had tried cannabis on one or more occasions and in 1975, 10.1 per cent. Thus the cannabis use pattern among Bergen youth does not appear to have changed much over the past two years and, generally, the percentage in Bergen is only half of its counterpart in Oslo. Also in Bergen the difference between boys and girls with reference to drug experiences has decreased in recent years, the last survey revealing that 10.9 per cent of the boys and 9.1 per cent of the gifts respectively had experimented with cannabis whereas the ratio in 1973 was 2 to 1. In the youngest age group a higher percentage of girls than of boys stated that they had tried cannabis. The development in Bergen shows a distinct decrease in the use pattern for the youngest boys. By far most of the young people report that they have used cannabis just once or a few times. In 1973, 31 per cent admitted to having tried the drugs more than 10 times against 25 per cent in 1975. The 1975 survey further showed a drop in the percentage of adolescents who had experimented with hallucinogenic drugs (amphetamines) as compared with the 1973 findings. On the other hand, the percentage of youth who had tried sniffing on one occasion or another has been constant also in Bergen, i.e. 9 per cent.
Record keeping on adolescent drug habits has been carried out also in Haugesund and Stavanger, towns located in the south-western part of Norway. Both surveys date from 1971. In Haugesund [ 32] , 7.5 per cent stated that they had tried cannabis. This percentage corresponds to that found in Oslo in 1970 and is somewhat higher than the percentage in Bergen in 1971. The Stavanger survey [ 8] comprises secondary school pupils only and, therefore, is not directly comparable with the other studies. However, viewed by age groups, the findings suggest a cannabis use rate of the same order as that found in Oslo in 1970. Other drugs, like the amphetamines, were used to a lesser extent. Six per cent and more of the Haugesund youth had tried sniffing on one or more occasions, while the rate was about 9 per cent at the same time in other towns. The above studies seem to show that use of drugs is a problem not specific to the Oslo youth.
Studies have been undertaken on drug use among students at the University of Oslo. In 1969 [ 12] , 4.5 per cent of the students had tried cannabis on one or more occasions. Over-all, 8 per cent of the students had experimented with one or more of the drugs in question at some point in their lives. Drug use among young men conscripted for military service in the Oslo area has also been investigated. It was found that in 1969, 8.3 per cent of the conscripts had tried cannabis at least once. A study on conscripts in the Oslo area in 1972 [ 1] showed that 9 per cent had used drugs more than 20 times and would probably continue to do so. Cannabis preparations were easily the most popular drugs. In 1973, 0.45 per cent of all Norwegian conscripts and 2 per cent of the conscripts in the Oslo area were diagnosed as drug dependents by the medical board [ 1] .
Quite as interesting as registration of the use pattern is registration of the attitude of youth towards drugs, more particularly to cannabis. At the first registrations in Oslo, about 3 per cent of the adolescents were of the opinion that cannabis ought to be sold freely. This figure rose to 6.5 per cent in 1971. Then it started to drop again. From the latest investigations a clear tendency to an increasingly negative attitude towards cannabis appears and an even stronger feeling against LSD and amphetamines. The young people were also asked whether they would try cannabis if they could do so without fear of being arrested. Whereas the earlier investigations showed that an increasing number of adolescents would like to try cannabis provided there was no risk of being arrested, there has been a clear downward tendency the last two years (to 9.7 per cent in 1975). In Oslo it appears to be fairly easy to get hold of cannabis in that more than half of the adolescents questioned stated that they had been offered the drug at one time or another. In Bergen the corresponding rate was 32 per cent.
A survey of use of sedatives in Norway during the last decade is included in a book published by the University Press (Universitetsforlaget) in 1974 [ 3] . The data quoted below are taken from this book.
Table 1 shows the total sales of pharmaceutical special preparations and of psychopharmaceuticals from Norsk Medisinaldepot to pharmacies.
Figure 1 shows the annual sales of "mild ataractic drugs", neuroleptics and anti-depressive drugs from Norsk Medisinaldepot, indicated in 24-hour dosages per inhabitant.
|
Year |
Total sales (current) (In million kroner) |
Sales of psycho-pharma-ceuticals yearly (current) (In million kroner) |
Psycho-pharma-ceuticals in percentage of total |
|---|---|---|---|
| 1958 | 53.2 | ||
| 1959 | 61.0 | ||
| 1960 | 66.2 | ||
| 1961 | 76.0 | ||
| 1962 | 85.9 | 9.2 | 10.7 |
| 1963 | 95.3 | 11.1 | 11.6 |
| 1964 | 104.8 | 13.5 | 12.9 |
| 1965 | 117.9 | 16.2 | 13.7 |
| 1966 | 137.0 | 18.8 | 13.7 |
| 1967 | 158.5 | 25.8 | 16.3 |
| 1968 | 179.3 | 29.9 | 16.7 |
| 1969 | 202.0 | 33.2 | 16.4 |
| 1970 | 226.5 | 37.4 | 16.5 |
| 1971 | 258.0 | 40.2 | 15.6 |
| 1972 | 290.6 | 38.4 | 13.2 |

Table 2 shows sales from Norsk Medisinaldepot in Norway in the year 1965 and the years 1970 through 1972 of barbiturates and other hypnotics, indicated in 24-hour dosages per inhabitant.
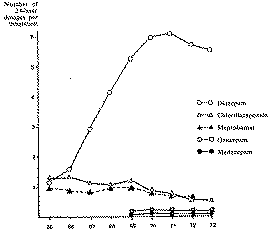
Finally, figure 2 lists the sales from Norsk Medisinaldepot of the separate "mild ataractics" expressed in 24-hour dosages per inhabitant.
As it becomes apparent there is considerable turnover of the "mild ataractics", especially of benzodiazepines, but there has been no sharp rise in the sale over the last few years. There has been a certain increase during the past 2 years, it is true, but this applies chiefly to metaqualone and nitrazepam preparations. Metaqualone was taken off the pharmacopoeia on 1 April 1975. As from the same date, the other drugs were placed in a prescription category where severer restrictions were applied. Over-all sale of mixed analgesics has decreased somewhat. Sale of narcotic drugs, that is drugs that are covered by the Convention on Narcotic Drugs, 1961, which belong to Group A in the current distribution regulations, has dropped [ 10] . This is assumed to be a consequence of the new control system introduced by the Directorate of Health, with electronic data processing of prescriptions. Since the introduction of this system on 1 July 1970,the number of prescriptions has fallen steadily. The last quarter of 1974, for instance, showed a decrease of 38 per cent relative to the same period in 1970 and as much as 64 per cent relative to 1969. Both total sales of narcotics and the number of prescriptions have fallen off distinctly during the period 1969 to 1975. On the basis of these data, it has been calculated that in 1974 an average of 1 per thousand of the country's over-all population had a 24-hour dosage of a narcotic drug. This figure does not seem alarmingly high and probably to a large extent represents a medically justified consumption which the health authorities would hardly want to query. The control instances that have been established show that older doctors tend to prescribe narcotic drugs to a greater extent than do their younger colleagues who appear to be more restrictive [ 10] . It looks as if information on the dangers involved in using dependence-producing drugs and the control systems that have been introduced have had a good effect. Use of sedatives appears to be at a fairly stable level in Norway, whereas use of legally prescribed narcotics seems to be on the wane.
|
1965 |
1970 |
1971 |
1972 |
|
|---|---|---|---|---|
|
Barbiturates
|
5.5 | 4.1 | 3.5 | 3.1 |
|
Other hypnotics
|
2.2 | 10.0 | 8.9 | 9.0 |
|
TOTAL
|
7.7 | 14.1 | 12.4 | 12.1 |
Nevertheless, the spread of sedative and hypnotic drugs is a problem that should not be overlooked. The tendency to abuse and dependence as regards these drugs in this country has appeared through consecutive registration of patients admitted to the University Psychiatric Clinic, Oslo, throughout a ten-year period [ 7] , [ 18] , [ 24] , [ 25] . Five per cent of all admissions during the period 1952 through 1961 were attributed to abuse of a sedative or hypnotic drug [ 24] . Up to 1955, barbiturates dominated the picture, then meprobamate gradually took over [ 7] , finally to be replaced by benzodiazepines after 1965 [ 18] , [ 25] . In the four-year period 1964-1967, 6 per cent of all patients in the hospital were addicts. Benzodiazepines were at that time the principal drug of abuse for 37 per cent of the registered addicts [ 25] . In 1968, when 12 per cent of the patients were drug dependents, the proportion primarily abusing benzodiazepines was 45 per cent [ 18] . Studies from other institutions, like Neevengarden Mental Hospital, Bergen, show corresponding figures. Thus, at the latter hospital, while 6.7 per cent of the patient population in 1971 were abusers of some dependency producing drug, no less than 77 per cent of them were addicted to benzodiazepines [ 9] . These Norwegian studies demonstrate that the proportion of drug dependents in a psychiatric hospital is on a par with that of a psychiatric clinic, and that benzodiazepines constitute the main group of dependency producing drugs among those admitted to psychiatric hospitals.
Whereas the number of morphine addicts seems to have remained fairly constant during recent years, the number of barbiturate and meprobamate abusers has dropped slightly. This is outweighed by a sharp increase in the number of benzodiazepines abusers, probably making the latter the largest group of addicts in Norway at present, as indicated in the in-patient studies reported above. Most important, multiple drug abuse characterizes the current drug scene to an ever-increasing degree. Young drug abusers frequently take barbiturates or benzodiazepines in addition to more typical drugs used by youth like cannabis or amphetamines. Heroin addiction is practically unknown in Norway.
The principles of treating drug dependence in Norway do not differ materially from those applied in other Western societies [ 21] . As a general rule, the drug dependent person should undergo a course of medical treatment. However, it often takes a long time for a person to admit to addiction and the need for help. In mild cases, a general practitioner is usually able to handle the case without referral to a hospital. Success in such treatment presupposes motivation on the part of the patient. However, often addiction is so far advanced before treatment is sought that no choice but hospitalization is left. In cases of long-term, chronic addiction it is deemed indispensable that the patient be hospitalized for some time. Norwegian drug dependents are usually voluntarily hospitalized in various facilities for treatment.
A patient may enter a somatic ward of a general hospital, but psychiatric institutions are usually preferred, partly because they provide several types of relevant treatment and partly because they can maintain a stricter regimen during the severe stage of withdrawal.
Psychiatric departments are becoming more numerous in Norway. There is practically one in each county attached to the central county hospital. Such wards are appropriate for first admissions. Ordinarily they treat a patient for a short time only, up to three, maybe even six, months. If treatment for a considerable period of time is needed, as is true in more severe cases of drug dependence, referral to a psychiatric hospital may be advantageous. This may be done pursuant to article 4 in the Mental Health Care Act of 28 April 1961. The patient then has to sign an agreement to the effect that he wants to be admitted, that he is willing to comply with the rules of the hospital, and finally that the provisions of article 4 have been made known to him. These provisions permit the hospital to hold him in the institution up to three weeks after he has requested in writing to be discharged. This is to allow the hospital a certain right of retention in case the patient should insist on being discharged during withdrawal. There are a good many psychiatric hospitals in Norway, one is usually available in each county. The divisions between psychiatric hospitals and psychiatric departments are gradually being removed.
The drug dependent may also apply voluntarily for admission to an alcoholism clinic which accepts narcotic dependents too for treatment. However, these places often suffer from a shortage of qualified staff, particularly physicians and psychologists. Finally, Norway has a special institution for treating narcotic patients. The State Clinic for Narcotics (Statens klinikk for narkomane), Hov i Land, to the author's knowledge is the sole institution in Europe that accepts nobody but drug dependents [ 29] .
Only rarely is involuntary treatment in a hospital enforced in Norway. Present laws governing compulsory commitment of narcotics addicts to an institution are [ 20] :
The Mental Health Care Act. In case there is doubt whether a patient suffers from a serious mental disorder, which is defined as a psychosis, the patient may be admitted to a psychiatric department or hospital pursuant to article 3 in the said Act. This article may be applied, e.g., for narcotic patients with whom the risk of suicide is deemed high. The hospital is then entitled to retain the person for observation against his will for up to three weeks. If the person is found to be mentally ill, he may be retained further pursuant to article 5 of said Act. Unless the patient is motivated for voluntary hospitalization, he must be discharged.
The Sobriety Councils Act. This act of 26 February 1932 for treatment of persons addicted to alcohol, is by amendment of 6 July 1956 made valid also for drug dependents. Pursuant to article 6 of this Act, alcoholics and narcotics addicts alike may, when a physician deems it advisable, be ordered to commit themselves to medical examination or treatment at an institution for one month, which period of time may be prolonged up to ninety days on the advice of the head physician involved. Finally, in case the drug dependent is grossly neglecting his duties towards family and community, the Sobriety Council may direct him to undertake treatment at an alcoholism clinic for any term not exceeding two years. In such instances the decision made by the Sobriety Council also has to be sanctioned by a judge who has to review the Council's decisions in passing such resolutions. Only rarely, however, are the coercive provisions of this law being applied.
Minor children may be hospitalized against their will pursuant to their parents' consent (parents' consent supposedly being required up to the eighteen-year age limit although most institutions will probably not be keeping children past their sixteen-year age limit). According to the Child Welfare Act, the Child Welfare Council may decide on deprivation of liberty up to the eighteen-year age limit.
By far the most frequent method of admission is for the drug dependent to come willingly to the psychiatric institution for treatment. It goes without saying that hospitalization often comes about after considerable environmental stress, and the patient frequently is forced by life circumstances to accept the hospital bed offered him.
Adolescent drug abusers may obtain treatment by either of the above two means. It should also be mentioned that in our two largest cities, Oslo and Bergen, and also in some medium-sized towns like Tønsberg and Kristiansand, there is a visiting out-patient service. In Oslo a special Field Service (Uteseksjonen) [ 28] is operating, in which social workers and milieu therapists visit places where drug-abusing adolescents congregate. They help make treatment arrangements in cases where care is deemed desirable or necessary. A similar programme is now available in Bergen too. Furthermore, special treatment programmes for young drug dependents exist in Oslo. These are a Pre-care Centre [ 6] and an After-care Centre, both working in co-operation with the State Clinic for Narcotics. Practising physicians and psychiatrists, of course, get their share of consultations, as do also psychologists.
Through funds granted by Parliament to the Central Council for Narcotics Problems in 1970, means were made available for promoting treatment services to adolescent drug dependents and for systematizing the body of experience. It was evident that considerable experimental and research work with different treatment models was required. Such experimental work was launched at the psychiatric hospitals of Dikemark, Oslo, followed by Neevengarden Hospital, Bergen, in 1971, and by Gaustad Hospital, Oslo, in 1973. In addition, similar enterprises were started at some clinic units like the Police Observation Unit at Ulleval Hospital, Oslo, the University Psychiatric Clinic, Oslo, and the State Centre for Child and Youth Psychiatry. Experiences gained from these places indicate that the size of a treatment unit should not be too large [ 17] , [ 21] , [ 31] .Treatment is based on either of two principles: the so-called, dispersion modeland the so-called concentration model.
In the dispersion model only one or two adolescents are accepted in the individual milieu therapeutic units of the hospital, and they are treated along with patients of any category of age and psychiatric disorder. The concentration model is operating in separate minor groups within a major treatment unit, the group usually consisting of about 10 patients who have a separate therapeutic team assigned to them [ 17] , [ 31] .
In our experience, the dispersion model has proved to be the one that fits in best in a psychiatric hospital. Using this, adolescent drug abusers make up but a small proportion in the various wards which must work according to active milieu therapeutic guidelines. Primarily two factors constitute the logical basis for the dispersion policy. One is the desire not to let the young drug dependents make up a strong sub-group within the ward and form their own sub-culture centered around drugs. According to Norwegian experience, young drug dependents have a challenging and provocative effect on the environment of the psychiatric hospital. It may be wise to take such defiance and provocation in small doses by mixing the adolescents with other patients, and not invite them to congregate into a strong and closely knit sub-group within the system. The other factor is that daily gathering with patients of other age groups and with other problems may prove beneficial to the young dependents. It has been found that young drug abusers are able to get correctives to themselves and to their problems from other adolescents, and no less from middle-aged and older people.
Systematized teaching and training of the staff attached to wards receiving young drug abusers have proved to be necessary. Such training is a pre-condition for a successful therapeutic set-up. Educational programmes are another precondition. Many of the young people have not completed their basic elementary schooling. In psychiatric hospitals that are to take in young drug abusers, therefore, there must be school facilities. Such have been established in Norwegian psychiatric hospitals pursuent to law.
Drug control must be possible, but then according to contract with the patients. Position to police and law system must be made clear. The young abusers must enjoy the same right to be protected under professional secrecy as do other patients. These young people are reluctant and distrustful towards helping agencies. Any treatment would be impossible if fear of being reported should prevent them from calling on the hospital. According to Norwegian experience, there is hardly any "danger of contagion" in housing young drug abusers in a psychiatric hospital. Social acceptance of drug abuse and drug ideology is reduced in the hospital by constant confrontation with adolescents who are hard beaten due to their drug abuse. However, it is important that these problems be worked on continuously with the staff members. A high activity level as regards milieu therapy, psychotherapy and group therapy is essential in a psychiatric hospital taking in young drug dependents. Also well-organized occupational therapy, school facilities, and not least recreational activities must be available. The latter should include a wide range of physical training and sports.
If the treatment is to be successful the hospital must provide adequate pre-care and after-care facilities. Furthermore, one should bear in mind that if the patient breaks the treatment contract and demands to be discharged this is no reason why the therapeutic team should abandon him. The patient should have a look at the hospital ward and be oriented about the treatment before admission. Motivation is considered to be of prime importance. It may be necessary with both one and two, and even more, contacts prior to admission. Good after-care contact is essential. A schedule for consultations ought to be made. However, experience shows that the young have difficulty in keeping scheduled appointments and appear on chance moments that suit them. Those who do not turn up have to be visited in their homes or the environments they are involved in.
According to Norwegian experience, the following requirements should be met if a psychiatric hospital is to succeed in treating young drug dependents in long-term therapeutic programmes [ 21] , [ 34] :
Afflicted persons should be treated in wards working along milieu therapeutic lines.
The hospital should provide educational opportunities and preferably also offer opportunities for some other kind of work or occupational training.
The hospital must have facilities for recreational activity and for self-expression far beyond what has been considered necessary for adult inmates in psychiatric institutions.
The hospital must have resources to commit itself to pre-care and after-care in an active way relative to these adolescents and their families.
The opening stage of such treatment programmes calls for continuous staff preparation and education about professional issues this group of patients raise.
The medical director of the hospital must have a favourable attitude towards, and a genuine interest in, the treatment procedure.
On appraising the situation in Norway, we conclude that the psychiatric hospitals in the country have to direct their efforts towards preparing a treatment offer for the young drug dependents. This concerns a group of people that society must not refuse to help. We have to realize that there are few, if any, other kinds of institutions that are better equipped for treating young drug dependents than are the psychiatric institutions. It would mean an extremely unfavourable development if the situation should so evolve that the psychiatric institutions would reject this group of patients without any better alternative being present. In the immediate situation the alternative is out-patient treatment by a Field Section (Uteseksjon) which exists in only a few places in our country and which has limited resources. Another alternative is penal institutions where treatment resources scarcely exist at all.
Whereas the other Nordic countries have chosen not to construct a special institution for treatment of narcotic patients, Norway opened its first institution of this kind in 1961: The State Clinic for Narcotics, Hov i Land. Experience from this programme demonstrates that such an institution meets a great need. The Clinic has acquired special know-how in treating drug dependents in closed as well as open wards, and has also served as a teaching institution for drug dependency problems [ 29] , [ 33] . The clinic has 36 beds. Three hundred and seventy-four patients were admitted during the period 1961 through 1967. Several scientific studies are undertaken at the clinic, inclusive of follow-up studies. The clinic also manages a pre-care and an after-care centre in Oslo.
In addition, some untraditional treatment models for young drug dependents have been developed. This includes a few collective enterprises which have been created in co-operation with the State Clinic for Narcotics or with some other psychiatric institution where young people are given responsibility and opportunities to do farming, forestry, or to become engaged in industrial activity. Experimental work which has been launched in this field looks most promising [ 33] .
In Norway there are no treatment facilities like Synanon, Daytop Village, or the like. A sceptical attitude to methadone maintenance treatment procedures prevails [ 11] . Methadone is applied to advanced morphine dependents during the withdrawal stage but only for a limited period. As mentioned above, there are very few heroin dependents in Norway.
Norwegian psychiatry has considerable traditions with reference to follow-up studies, more particularly personal follow-up studies. The small Scandinavian countries have a scarce and well-registered population which makes it possible to trace practically 100 per cent of the patients. This represents a very real advantage. There follows a review of follow-up investigations, first on more traditional, then on juvenile drug abuse.
Retterstöl and Sund [ 24] did the first personal follow-up study on drug addicts in Norway. During the years 1952 through 1961, about 5 per cent of all patients admitted to the University Psychiatric Clinic, Oslo, were classified as drug dependents. The follow-up study comprises 152 patients who were personally re-examined, mostly in their homes, after an observation period ranging from 1 to 10 years. Eighteen patients had died during the period of observation and 122, that is 92 per cent of the survivors, were personally followed up. Of central data may be mentioned that for these patients the drug abuse had lasted from 1 to 25 years. Only in 5 to 10 per cent of the cases had painful illness originated the drug habit. For the remaining, personality deviations, neuroses, or serious mental disorders appear to have triggered the drug habit. On follow-up, a third of the patients had stopped misusing drugs. As could be expected, this rate was higher for habituated than for addicted patients, 43 per cent and 23 per cent respectively. Barbiturate abusers had managed to lay off the drugs to a greater extent than the morphine abusers. The tendency to switch from barbiturate to meprobamate during the observation period was very distinct. Almost three quarters of all patients had maintained the same job throughout the period. The percentage was much the same for morphine and barbiturate abusers. Nearly two thirds had not at all been unfit for work. The figure was most favourable for habituated patients. Two patients had fallen very low socially and were in a severe state of social deterioration. Eighteen per cent had attempted suicide during the observation period. The following were found to be favourable prognostic factors: harmonious childhood conditions, relatively unremarkable personality, previous good work adjustment, none or brief previous unfitness for work, no alcohol problems, below 30 years of age, short duration of abuse. Finally, habituated patients had fared distinctly better than had the addicted.
Waal has presented a preliminary follow-up study on 40 young drug abusers treated at the State Clinic for Narcotics [ 33] . These were re-examined in 1973 after an observation period of upwards of 4 years. At the last examination it appeared that 14 patients had not resorted to any intoxicant the last year, 6 reported a sporadic and controlled consumption of hash, 8 multiple drug abuse predominated by hash, 3 misused opiates or central nervous system stimulants, and 7 were definitely dependent on several drugs. Twenty, that is half of the patients,
Drug dependency in Norway 39 were quite or nearly intoxicant-free. For 18 patients (45 per cent) the misuse status was judged to be satisfactory and the patients were in full work.
Westin [ 34] re-examined a smaller group of patients which is included in Holsten's material mentioned below, after one year. Holsten did a personal follow-up investigation of 91 patients treated at Neevengarden Hospital, Bergen, because of drug dependence [ 15] , [ 16] . The treatment was carried out according to the dispersion model. The observation period ranged from 1 to 4 years. On follow-up, 76 per cent of the patients did not misuse drugs, 67 per cent had not done so the last year, and 41 per cent not for the past 3 years. Thus it looks as if the number of drug-free persons augments with time. Thirty-eight per cent of the patients were drug-free, had a regular work situation, and an ordered housing situation.
Holsten [ 14] likewise investigated the incidence of "flashbacks" and found that 39 per cent of the admitted patients had experienced such phenomena and that they might go on for years. Also further course was somewhat less favourable for the drug abusers who had experienced flashback phenomena during hospitalization [ 16] .
Stang's follow-up study [ 28] comprises a material of patients treated by the Field Section, Oslo, that is patients encountered or seeking help outside institutions in Oslo. The material includes 100 youths with a heavily charged background. After an observation period of at least three years, 4 patients had died, 3 were living abroad, and the remaining patients were followed up. The development profile showed that approximately 40 per cent had improved throughout the observation period, whereas 15 per cent had slipped downhill with increasing abuse, legal conflicts, and social problems. Upwards of half the patients were in better shape physically than they had been when last seen. At the follow-up examination, 44 patients were drug-free, 29 of whom for more than a year. Early loss of parents, broken homes, insecure childhood conditions, and stay in an orphanage proved to be factors indicative of unfavourable development, while stable childhood conditions with united parents pointed in a favourable direction.
Norwegian personal follow-up studies suggest that the course is more favourable for adolescent drug dependents than for older, more traditional, abusers. One reason for this might be that it has been "in"to use drugs; that many of the young people may have experimented with drugs out of curiosity and then been lucky enough to get under treatment before the behavioural pattern had stiffened. Another reason might be that many of the adolescents caught by the drug habit may have been immature as to personality structure and may have been confronted with a school or life situation they were unable to cope with. In time they mature, in part spontaneously, in part subsequent to treatment and teaching programmes they go through. This seems to imply that the potentials which despite all are inherent in the young drug dependents have been grossly underrated.
After the flood of adolescent drug dependence had reached our shores a Central Council for Narcotics Problems was set up by the Government in 1969. This was composed of one representative from each of the following ministries: Social Affairs, Justice, Church and Education, and Finance and Customs [ 20] .
This Central Council serves as a consultative body to the Government. Four sub-committees under the direction of the Council are appointed. Each of them works on a separate aspect of the narcotics problem: [ 1] an interdisciplinary treatment committee; [ 2] an information bank; [ 3] a research group, and [ 4] a lecturing and instructional pool which is to co-ordinate the educational task.
There is no doubt that the Central Council for Narcotics Problems has played an important role in preventing adolescent drug dependency in Norway. The Central Council for Narcotics Problems is granted funds by Parliament. Over the past several years they have been receiving 3.5 million Norwegian Kroner annually to support their work. Among other things, the Central Council has taken the initiative in establishing treatment units to try out different types of treatment models and to organize prophylactic measures on the national as well as the local level. Treatment models described above with the development of dispersion and concentration models are the result of central planning by this Council. The Information Bank of Narcotics Problems has now been operating for five years and has been issuing approximately a hundred information articles each year, the number being increased the last two years, addressed primarily to the Norwegian medical profession and published in the Journal of the Norwegian Medical Association, copies of which are sent to all Norwegian physicians [ 20] . All members of the Council and also all members of the liaison committee in each county receive their copies, as do also hundreds of Norwegian doctors, school directors and social centres throughout the country. In this way, efforts are made to keep the medical profession and also interdisciplinary groups informed about developments within narcotics problems, inclusive of size of the problem, treatment, and prophylaxis. Excerpts of international literature of interest in this field are distributed through the Bank. Endeavours are also made to reach the school system by lectures and educational work. Instruction on narcotics as well as alcohol problems has become part of the schools' curriculum throughout the country and special teaching material on the topic has been prepared by central and local workers.
An important prophylactic step initiated by the Director of Health in co-operation with the Central Council for Narcotics Problems is the appointment of a liaison committee in each county, the members of which include local authorities representing the police, health and social services agencies, and the educational sector. The liaison committees co-ordinate county-level work on narcotics problems and meet centrally from time to time for discussions and mutual exchange of information. The liaison committees have their own budgets. Central information is distributed to the county committees by the Information Bank and by the Central Council for Narcotics Problems. Preventive work of great value is carried out locally under the direction of these committees.
The Nordic countries collaborate on narcotics problems, and in the past years several joint Nordic seminars on this topic have been held under governmental auspices. A Nordic report has also been published by the Nordic Council concerning narcotics research [ 19] . Furthermore, a special liaison group has been set up with membership including high governmental officials from each of the Nordic countries. This group meets regularly to discuss narcotics problems and tries to co-ordinate measures taken in the four Nordic countries. Iceland is not yet represented in this group.
Such control is systematically carried out in Norway. From 1 July 1970, an effective control system for prescription and consumption at physician/patient level has been in operation in Norway, in that all prescriptions classified under Group A in the current distribution statutes and sold in pharmacies have been processed by electronic computer at Norsk Medisinaldepot. The quarterly reports from the electronic data processing are checked by the Ministry of Social Affairs. This ensures strict control of physicians and their prescription of drugs. In cases where a doctor's prescriptions appear blameworthy or where there is reason to suspect that he himself is dependent, he will be asked to explain the matter to the Director of Health. Should he be unable to give a satisfactory explanation for his prescriptions, he will receive a warning. He will know that he is under continued surveyance, and this fact will often make him change his ways. If not, the case may be brought before the Control Board for physicians' prescription of narcotics. The doctor in question is entitled to voluntarily renounce his right to prescribe drugs instead of having the case tried by the Control Board. If a case is brought before the Board, the physician will automatically lose his licence to prescribe until the Board has reached a decision. During the 5-year period that has elapsed since electronic data processing of narcotics prescriptions was introduced, 26 physicians have renounced their right to prescribe narcotics for periods ranging from one to two and up to ten years. Practically without exception, these physicians have been drug dependents themselves. If the register shows that a patient is seeing several doctors in order to get hold of large quantities of narcotics, all prescribing doctors will be notified by the Director of Health. This may mean that the treatment is canalized to one particular physician who will then be responsible for the treatment of the drug dependent and will arrange to have all prescriptions of drugs for this patient go through one and the same pharmacy. The aim is to get the patient's consumption under control with a view to wean him from his habit, if necessary by admission to a suitable treatment institution. Electronic data processing of all prescriptions for dependency-producing drugs is looked upon as an important prophylactic step.
Theft of prescription pads and physicians' stamps as well as falsification of prescriptions has become increasingly frequent in recent years. Special forms for prescription of narcotic drugs were introduced in 1976.
In Norway, the control of preparations that are to be marketed is very strict. All drugs that are to be put on the market in the form of special preparations have to be approved by the Specialist Board, made up of the Director of Health, two medical and pharmaceutical authorities. The over-all system imposing import and export licences and control of home production, sale, and consumption of dependency-producing drugs is scrupulously checked through the sales statistics of Norsk Medisinaldepot. By this means, the health authorities are able to survey the distribution of narcotics and other dependency-producing drugs. Should the sale of one drug or another increase disproportionally more than seems warranted for medical reasons, the Directorate of Health may consider introducing further restrictive measures. This may be done, for instance, by striking certain preparations from the register or by imposing specific licence regulations as has been done for central nervous system stimulants.
These are relatively strict. Unless obtained upon prescription, use of dependence-producing drugs is prohibited. This applies to cannabis, among others. The distribution of narcotic drugs is regulated by a licence system. Up to 1968, infringement of the Statutes was punishable by imprisonment for a term not exceeding two years. This penalty was low by international standards. The Criminal Law Council suggested in its report for 1967 that the maximum penalty be increased to imprisonment for five years. Parliament, however, set the upper limit for imprisonment to six years which may reflect public opinion relative to crimes of this kind. In 1972, the maximum penalty was increased to ten years' imprisonment by Parliament. This Order is still valid at present. The same maximum penalty is applicable in Sweden and Finland. The hardest punishment is, of course, reserved for gross criminal actions done for profit. Among Norwegians there is general agreement that serious narcotics crimes merit severe measures. Remonstrances to the punitive measures have special application to drugs where usealone is punishable too. This has particular reference to cannabis preparations as experience has shown that a number of young people encounter this drug more or less accidentally. A strict penal legislation may entail that using a drug once or a few times is made a criminal offence and hence cause criminalization of a pattern which neither the over-all population nor the group itself regards as a crime. Discerning practice of the law will be decisive for whether or not a legislation like ours can be maintained. At present the strict Norwegian legislation is strongly supported by the people.
Another important prophylactic measure is establishment of youth clubs around the country. These clubs help organize more meaningful leisure pursuits for adolescents who seem to have difficulty adjusting to home and school. In most towns special municipal organizations co-ordinate work for youths. The establishment of field service units which are also organized by the community in major Norwegian cities may also be viewed in part as prophylactic measures since staff members of this service both contact drug dependents at an early time and seek out non-drug-using adolescents who mingle with the abusers, therefore constituting a high-risk group. These field service units have been mentioned above.
In Norway strong emphasis is placed on educational work. This is directed first and foremost toward physicians and interdisciplinary groups of field workers. The educational campaign is organized by the Central Council for Narcotics or by the liaison committees in the counties and has, without doubt, been important for the relatively strong stand against drug use in Norway.
Research into narcotics problems represents another important prophylactic measure. A good deal of research has been done in this field. The work has been practically directed, in part sociological in the form of field studies and epidemiological work elucidating use of dependency producing drugs, in part clinical including evaluation of treatment and systematic follow-up studies of clinical material as described above. Less basic research is pursued. There is close collaboration between the Nordic countries within the scientific sector. To further this collaboration, the Nordic Joint Committee for Narcotics Research has suggested to the respective Governments that a special Nordic collaboration agency be instituted. This has now been established under the name of Nordic Drug Research Institute (Nordisk Drog Forskningsinstitutt). The Institute is situated in Oslo, affiliated to Gaustad Hospital. From this institute one is in touch with the Nordic milieux that engage in research projects pertaining to narcotics problems.
In conclusion, it should be mentioned that endeavours are made to co-ordinate prophylactic efforts and treatment schemes by arranging frequent seminars for "key personnel" on both national and local levels. During the last three years, also on Nordic levels. This is done to exchange information between persons working with drug dependents, primarily representatives from health and social service agencies, the police, and schools.
The secondary prophylaxis consists mainly of visiting out-patient service, among other things in connexion with the Field Services in the various cities which employ social workers, child welfare educators, milieu therapists, psychologists, doctors, and volunteers.
The tertiary prophylaxis is closely associated with treatment, after-care, and rehabilitation and has been accounted for under "Treatment" in the present paper.
Lastly should be mentioned that little opposition has been voiced against the official narcotics policy which seems to be widely accepted throughout the nation. At the moment the narcotics situation appears to be fairly well under control in Norway.
J. Aaseth, B. Rekdal and A. Sund. Utbredelse av stoffbruk hos unge menn i Norge i 1972-73. Nord. Psykiat. T ., 29, 271-278, 1975.
002O. Arner. Stoffbruk blant ungdom i Oslo 1968-1970 og i Tønsbergdistriktet 1970. Statens institutt for alkoholforskning, Oslo, 1971.
003A. Bakke, A. Johnsen, H.E. Rugstad and P. Sundby. Bruk av beroligende midler i Norge. Universitetsforlaget, Oslo, 1974.
004B. Bergersen. Oslo-ungdoms bruk av marihuana og hasjisj. T. samfunnsforskn., 9, 208-232, 1968.
005S. Brun-Gulbrandsen and B. Bergersen Lind. Marihuana og hasjisj. Holdninger og bruk. Universitetsforlaget, Oslo, 1970.
006D. Coucheron. Statens Forvernssenter i Oslo. Arsrapport 1972. Oslo, 1973.
007L. Eitinger, N. Retterstöl and A. Sund. Meprobamat. Tilvenning til og vanemessig behov for preparatet. T. norske lœgeforen, 80, 914-917, 1960.
008A. Flo, E. Larsen, ?. Stromme-Rasmussen and A. Vorland. Rusmiddelbruk blant ungdomsskole-elever i Stavanger hosten 1971. Stavanger, 1972.
009G. Haaland. Stoffmisbruk blant hospitalisert psykiatrisk klientell. Psykologisk institutt, Universitetet i Oslo. 1971.
010I.K. Halvorsen, T. Haraldseid and B. Joldal. Narkotikaforskrivning og forbruk i Norge 1970-1974. T. norske lœgeforen, 95, 1765-1770, 1975.
011O. Hallgrimsson. Misbruk og forgiftning med methadon. T. norske lœgeforen. 17, 1144-1145, 1974.
012L. Hjort. Cannabismisbruk blant studenter i Oslo 1969. Statens institutt for alkoholforskning, Oslo, 1971.
013L. Hjort and O. Irgens Jensen. Bruk av stoffer, alkohol og tobakk blant ungdom i Oslo 1968-1973. Statens institutt for alkoholforskning, Oslo, 1973.
014F. Holsten. "Flash-backs" - senreaksoner etter bruk av LSD og Cannabis hos 78 stoffmisbrukere. T. norske lœgeforen, 94, 2070-2077, 1974.
015F. Holsten. Unge stoffmisbrukere - videre skjebne etter behandling. T. norske lœgeforen, 95, 171-177, 1975.
016F. Holsten. Stoffmisbrukere: Behandling og videre forlop. Gold Medal of H.M. The King of Norway. University of Oslo, Oslo, 1975.
017J. Jorstad. Behandling av unge stoffmisbrukere i et terapeutisk samfunn. T. norske lœgeforen, 18, 1367-1373, 1971.
018A.O. Lunde and O. Ropstad. Misbruk av lette ataraxia. Nord. Med., 655-658,1970.
019Narkotikaforskning. Rapport fra det nordiske fellesutvalg for narkotikaforskning til de nordiske lands regjeringer. Nordisk Rad, Nordisk udredningsserie 11/70, Stockholm, 1970.
020N. Retterstöl. Stoff og alkohol. Bruk og misbruk. Universitetsforlaget, Oslo, 1976.
021N. Retterstöl. Principles for treatment of adolescent drug dependents in psychiatric hospitals. In: Skandia International Symposia: Drug Dependence - Treatment and Treatment Evaluation, pp. 97-105. Almquist & Wicksell, Stockholm, 1975.
022N. Retterstöl. Use and abuse of dependency producing drugs in Norway. J. Drug lss., 5, 22-32, 1975.
023N. Retterstöl. Missbrauch von Drogen in Norwegen. Fortschr. Neurol. Psychiat., 43, 347-358, 1975.
024N. Retterstöl and A. Sund. Drug addiction and habituation. Universitetsforlaget, Oslo, 1965.
025N. Retterstöl and O. Ropstad. Misbruk av lette ataraxia. Nord. Psykiat. T., 23, 477-492, 1969.
026Statens institutt for alkoholforskning: Narkotikaundersakelse i Bergensdistriktet. Pressemelding, 1971, 1973 og 1975.
027Statens institutt for alkoholforskning: Narkotikaundersakelse i Oslo 1975. Pressemelding, 1975.
028H.J. Stang. Ungdom i drift. Universitetsforlaget, Oslo, 1976.
029A. Teigen. The Hov treatment unit and the Oslo Half-Way House. In: Skandinavia International Symposia: Drug Dependence - Treatment and Treatment Evaluation, pp. 116-126. Almquist and Wicksell, Stockholm, 1975.
030A Teigen. Erfahrungen in Skandinavien (nichtalkoholische Suchte). In: W. Stein-brecher and H. Solms: Sucht und Missbrauch., pp. 124-135. Thieme, Stuttgart, 1975.
031P. Vaglum and B. Bjelke. Unge stoffmisbrukere i en psykiatrisk avdeling. T. norske lœgeforen, 93, 7-12, 1973.
032V. Vandvik. Stoffbruk blant ungdom i Haugesund 1971. Statens institutt for alkoholforskning, Oslo, 1972.
033H. Waal. Behandling av unge stoffmisbrukere i specialklinikk for narkomane. Nord. Psykiat. T., 29, 3-20, 1975.
034S. Westin. Behandling av unge stoffmisbrukere i et psykiatrisk sykehus. T. norske lœgeforen, 93, 1662-1668, 1973.