I. Description of program and patients3
Author: Robert OSNOS , David LASKOWITZ,
Pages: 31 to 46
Creation Date: 1966/01/01
I. Description of program and patients 3
Introduction
Greenwich House, a community center in the Greenwich Village section of New York City, became concerned about the increasing problem of drug addiction in the neighborhood in 1962. It turned for advice to New York University, which is also located in Greenwich Village. The two organizations jointly applied to the National Institute of Mental Health of the United States Public Health Service for a mental health grant to finance a treatment and research program for drug addicts, to be based in Greenwich House. The grant was approved and the program, called the Greenwich House Counseling Center, was initiated in May 1963.
In its first 20 months the Greenwich House Counseling Center provided treatment for 441 drug users.
The present paper and the one entitled "A Counseling Center for Drug Addicts; II, Analysis of Results", report on the Center's experience and results during the first two years of operation. The present paper reviews the treatment of drug addiction in the United States at it pertains to the Counseling Center; describes the Center's programs and the patients who were treated; discusses case finding, community relationships, treatment of families and group treatment techniques.
The purpose of the research was to determine which patient and treatment characteristics are related to the degree of involvement in treatment and concurrent changes in adjustment. Selected factors were identified and correlated with an attendance index, which was a measure of treatment involvement, and a series of adjustment scales. From these data certain implications were derived regarding the prognostic-significance of patients' background regarding amenability to treatment and future adjustment.
1Dr. Osnos is presently Director of Psychiatry (Courts), New York City Community Mental Health Board.
2Dr. Laskowitz is presently Director of the Drug Abuse Service of the Lincoln Hospital Mental Services in New York City.
3The second and concluding part of this study will be published in a subsequent number of the Bulletin.
The authors are deeply indebted to the staff of the Greenwich House Counseling Center, all of whom participated in the treatment and in the gathering of the research data. They are: Mrs. Mary Wilbur, Mr. Thomas Connor, Mr. Arthur Pierson, Mr. Peter Quartaro, who are social workers, and Mrs. Susan Taylor, who is a public health nurse. The Center was guided by a steering committee consisting of Dean Alex Rosen of the New York University Graduate School of Social Work, Professors Isidore Chein, Sidney Roth and Albert Somit of the New York University faculty, and Dr. Maxwell Powers, Director of Greenwich House. The indispensable secretarial help was provided by Miss Lydia Williams and Mrs. Barbara Godett.
Treatment of drug addiction in the United States
During the past four decades narcotic addicts, in the United States, have generally been treated in specialized facilities designed for them.
Until 1952, the only hospitals for addicts were the United States Public Health Service Hospitals in Lexington, Kentucky, and Fort Worth, Texas [ 13] , [ 17] , [ 24] . The Lexington Hospital found that most of the addicts who came there voluntarily remained only long enough to be withdrawn from narcotics and did not use the hospital's rehabilitative resources. As the two hospitals enlarged their programs and acquired further experience, their staffs repeatedly emphasized that hospital withdrawal and treatment in a drug-free environment, including vocational rehabilitation and psychotherapy, were only the initial stages of rehabilitation and had to be followed by care in the addict's own community [ 13] , [ 19] . Unfortunately, even those municipalities which had a severe problem responded only in a token fashion. Treatment programs in Chicago and Detroit were hampered by lack of support from local government and various helping professions [ 3] , [ 22] .
In 1952, Riverside Hospital, operated by the New York City Department of Hospitals, was opened for the treatment of adolescent addicts [ 14] . It corrected some of the shortcomings of the federal hospitals. A public health law provided a civil commitment procedure, so the patients could not leave at will. An after-
care clinic housed in a general municipal hospital was established and it was staffed by the same staff who worked in Riverside Hospital to provide continuity of patient care. However, the hospital soon faced severe problems. Contrary to general expectations adolescents were found to be more difficult to involve in treatment than older addicts [ 1] , and because the after-care clinic was not located in the immediate community of many of the patients, it could not cope adequately with the stress of transition from hospital to the community. The hospital was subject to continuous public controversy and it finally closed in 1963.
During the past ten years, most of the important developments in the treatment of addiction have occurred in New York City, which is reported to have between 25,000 to 30,000 addicts. This is about half of the known narcotic addicts in the United States [ 25] . Voluntary programs, many sponsored by church organizations, started to provide counseling, job referrals, and religious support right in the addicts' communities. Their efforts were also hampered by insufficient funds and lack of professional staff. However, they made an enormous contribution; they alerted the general public to the problem and they demonstrated that addicts would seek help if it were provided by persons they could trust and who were not closely identified with authority and law enforcement.
Concurrently the Demonstration Center of the United States Public Health Service in New York City developed outpatient techniques for treating addicts. It also educated public agencies, such as the Department of Welfare and the Division of Vocational Rehabilitation, to accept the special needs of addicts [ 4] . The Center also found that though immediate results of treatment were poor because of the high relapse rate, with the passage of time a gradually increasing number of its patients were able to abstain from drugs.
Another outpatient project in the late fifties was organized by the Postgraduate Center for Psychotherapy [ 16] . Trained psychotherapists treated addicts privately and found some of them could be treated as other psychiatric patients with a degree of success.
Hospital services for addicts were also expanded. In 1958, the New York City Department of Hospitals opened special detoxification wards within its general hospitals. One of these also provided extensive after-care.
The Volker-Metcalf law passed by the New York State legislature in 1961 created separate units in state mental hospitals and an after-care clinic for narcotic addicts. Some of the patients in these units are civilly committed instead of being sentenced for drug-connected crimes. The terms of a commitment are compulsory hospitalization and after-care treatment.

The counseling process: addicts being interviewed by a psychiatrist (above) and a social worker (below)
In summary, in the early 1960s hospital services were provided either by municipal or state hospitals, and outpatient treatment by governmental agencies or interested individuals. Nongovernmental outpatient services were neither fully professionally staffed nor adequately financed.
The Center was intended to fill this gap. Its purpose was to determine what could be accomplished by a wholly professional multi-disciplinary staff that was part of a nongovernmental setting which addicts would be more apt to trust, since it was less indentified with authority and law enforcement. In addition, the greatest break-throughs in other social problems have been made when experienced personnel could work in flexible administrative settings which encouraged experimentation.
Rationale for specialized treatment services for drug addicts
It is necessary at this point to summarize the advantages and hazards of treating drug addicts in special programs, rather than in settings which also serve other kinds of patients.
The principal argument for specialized services is that addicts present many unique treatment problems. If all the patients are drug addicts the staff is able to acquire knowledge and experience in various aspects of drug addiction, so it can cope with these problems. Since addicts are usually difficult and unrewarding patients, the staff of a general agency, who is not knowledgeable in addiction, is inclined to avoid them. In a specialized setting this does not happen.
A staff which is expert can deal more efficiently and effectively with its patients. Also it can develop special administrative procedures which are responsive to their unique difficulties. In this paper several examples of these are given, including security measures to protect against theft, and simplified intake procedures.
Another reason for specialized services is the prevention of contagion. It is generally agreed that drug addicts try to introduce others to drug use. Originally this was believed to be for financial gain to develop potential buyers of drugs. This view is now discarded, since drug addicts are usually introduced to drugs by their friends; it is probable that they want to share a pleasant experience, or perhaps on a deeper level, want others to share their suffering [ 5] .
A related issue is the disturbing effect of the presence of drug addicts on non-drug users. All one has to do is to ride in the same subway car with a highly intoxicated addict and observe the reaction of the other passengers. The intoxication is usually attributed to alcohol and there is the ensuant fear of violent behavior.
Finally, drug users may be more apt to accept treatment in a specialized setting where they know they will be understood and accepted. They also know they will not have to hide or defend their drug use and explain behavior that may seem particularly strange to an uninformed person.
One of the disadvantages of a specialized setting is that it encourages addicts to congregate. They can then stimulate each other to drug use; the less experienced ones may acquire new information from the older drug addicts and the association may enhance alienation from non-users.
There is a social stigma associated with treatment at a known center for addicts. For instance, if a patient were referred by the Center for employment he loses the option of disclosing to a potential employer that he was or is an addict. This is important because there are doubtless certain jobs which addicts can fill which would not be offered to them if the employer knew that they have used drugs. Another disadvantage of specialized settings is that the staff can become too accepting of certain addict patterns. For instance, voluntary patients come back many times at the Lexington Hospital. Occasionally, a patient who has been there many times, returns and he is greeted like a long-lost friend by some of the staff, particularly if he has a vocational skill useful to the institution.
All these points were kept in mind when planning the program of the Greenwich House Counseling Center, since it is a specialized program, but in a setting where other kinds of clients are present.
Description of Greenwich Village
Greenwich Village is one of the best known neighborhoods in the world. For many years it has been a haven for artists dedicated to experimentation and creativity, somewhat in the tradition of the left bank of Paris. The Village is also referred to as "Little Italy" since many of its residents are first and second generation Italians.
Since the end of World War II the character of the Village has changed. It has become an expensive and fashionable residential neighborhood. The presence of many experimental theatres ("Off Broadway") and restaurants has made it popular with tourists. It has also attracted many young people who have artistic pretentions, but insufficient talent and self-discipline to support their aspirations. As is to be expected some of them espouse unrestrained individuality. They have been called "Beatniks" [ 11] .
The following are among the social ingredients in Greenwich Village: an Italian population which tries to maintain its way of life, and resents encroachments of all kinds; wealthy people who consider the neighborhood fashionable; genuinely creative persons; many non-conformists, and a large number of transients and tourists. The conflicts between these groups are expressed in fervent political contests between "old line political bosses" and "reformers". One of these was eloquently dramatized in a recent play, "A Sign in Sidney Brunstein's Window" [ 8] .
Drug addiction in Greenwich Village has two sources. In the early 1950s a group of Italian and Irish youths started using marijuana and heroin. There was a great deal of community concern with the problem. However, only a few new addicts were added to the original group. Most of those who were already using these drugs continued to do so, through some died, some moved away and a small number stopped.
The other type of drug use in Greenwich Village involves the use of non-opiates such as marijuana, amphetamines, barbiturates and hallucinogens by the "Beatniks". These users are generally aware of the addic- tive liability of heroin and limit their drug use to other drugs which are cheaper and less apt to lead to conflict with the police. 4 They feel that these drugs enhance their creativity and self-understanding. Unlike heroin addicts, they do not experience their drug use as a problem and they feel they can stop at will.
We expected that we would gain a better understanding of non-opiate drug abuse through our program.
Description of Greenwich House
Greenwich House is a six-story building in the heart of Greenwich Village. It is operated as a non-profit organization by a Board of Managers who are a non-salaried group of prominent citizens. The Greenwich House Counseling Center was entirely financed by United States Public Health Service Grants MH-01157-01-02-03, from May 1963 to August 1965. It is presently financed by the Division of Narcotics, New York State, Department of Mental Hygiene, and the New York City Community Mental Health Board.
Its programs include after-school activities, adult education classes, a nursery for children of working mothers, a visiting nurse service, and a variety of community meetings. Two other buildings house a well-known music school and a pottery school.
The Counseling Center has a suite on the third floor consisting of seven interview rooms and a small secretarial waiting-room. It is furnished informally so as to be non-institutional in appearance. The waiting area is intentionally kept small so as to discourage patients from congregating. Another room on the fourth floor is used for group activities.
We did not want our patients to roam through the building. We asked them to stop at the switchboard on the main floor and use the elevator; the elevator operator was instructed to see that they went directly into the Counseling Center. Whenever these rules were relaxed, as when the building was being renovated, patients were found in other parts of the buildings, e.g., using an empty bathroom to take drugs. There were also a few thefts of such items as a film projector and a typewriter. Probably these were done by patients who were familiar with Greenwich House and felt free to wander around.
Some of the patients congregated in the lobby on the main floor, particularly around 5 p.m. when mothers were picking up their children from the nursery. Since the patients were usually intoxicated and dishevelled, the Center's director asked them not to be there atthat time. They promptly accused him of being biased and rejecting. He pointed out that because they were under the influence of drugs they were not aware of how frightening and unsavory they looked, especially to people who know little about addiction. Furthermore, if they persisted there would be a community protest and the Counseling Center might have to close. This realistic approach was accepted and they stopped congregating. Throughout the two years there was minimal open resentment from other participants in Greenwich House activities and no community resistance to the program. 5
The staff of the Counseling Center was chosen to represent various professional disciplines, since we felt that different professionals could provide special skills to deal with the treatment problems. The director (Robert Osnos, M.D.) is a psychiatrist who has had diverse experience treating addicts. He is the Center's administrator and supervises the rest of the staff. The assistant director (David Laskowitz, Ph.D.) is a clinical psychologist who has a similar background. He is in charge of the Center's research and evaluative program.
The remainder of the professional staff consists of two social case-workers, two social group workers and one public health nurse. Only one of them has worked with addicts in the past but all have had extensive experience with lower socio-economic class patients and with disturbed adolescents.
The whole staff, including the two directors, participates in all aspects of the program: treatment, community activities, research and evaluation. This is done because the maintenance of staff interest in all aspects of the program is important for their morale. Poor morale can quickly become a serious problem when treating difficult and frequently unrewarding patients.
Case finding
We adopted the broadest possible definition of drug addiction for the following reasons: recent increase in the abuse of non-opiates [ 25] ; our own experience that there is no reliable way of distinguishing between the drug user and the drug addict; the observation that the opiate user turns to other drugs as occasional or permanent substitutes.
Using Jaffee's suggestion [ 10] we defined as a drug user and accepted for treatment anyone who used any drug in amounts greater than medically indicated. The only exception was made in the case of exclusive abuse
4In the United States, the importation, manufacture, sale and possession of heroin is illegal and most narcotics control efforts are concerned with enforcing this.
5Many fine programs for addicts have had to cease operation because of vociferous objections originating from individuals who had realistic and sometimes unrealistic concerns about congregation of addicts in their neighborhoods.
of alcohol. We felt that alcoholism presents different treatment problems than drug abuse due to the medical complications of chronic alcoholism.
Our hypothesis was that in spite of our broad definition of drug abuse the vast majority of our patients would be heroin addicts and only on rare occasions would a patient be referred to us who should not be treated as a drug user. 6 Thus, we saved ourselves and the referring agencies a great deal of time which would have been otherwise spent deciding if a particular individual was eligible for treatment.
Initially, we intended to restrict our work to drug users who resided in the Greenwich Village area. We soon discovered that there were not enough users in the area to keep us busy. Consequently, we accepted for treatment patients who resided anywhere in New York City. However, we particularly encouraged referrals from the neighborhood and our efforts at case finding were concentrated in the Greenwich Village area.
Case finding was carried out in essentially two ways:
Canvassing known addicts in the neighborhood. We hoped to obtain the names of all reported addicts in the neighborhood from the registry of addicts of the Office of Narcotics Coordinator. These data are unavailable for administrative reasons. However, we were able to get from other agencies the names of 55 addicts and the public health nurse sought them out. Forty of these could not be located or had moved. The 15 whom she found eventually came to the Center and many became regular patients.
Becoming known to other agencies. The staff visited 70 agencies to describe the Center to them. These included hospitals, welfare and health centers, probation and parole departments, other settlement houses, churches and non-professional neighborhood groups. We also mailed a description of the Center to all physicians, lawyers and neighborhood groups listed in the Greenwich Village Directory. The letters produced minimal response; in contrast, our visits to the agencies stimulated interest in the Center as evidenced by referrals of patients, return visits and requests for additional information.
Our case finding procedures resulted in a progressively increasing number of new patients seen at the Center (figure1). The first 200 patients were referred from 50 different sources. Also, we reached a progressively greater proportion of drug users who had no counterpart treatment experience. A quarter of the first 100 patients had no prior treatment; however, almost half of the subsequent patients were in this category.
Selection of treatment modalities
There were three major considerations in the selection of treatment programs: we needed some indication that a particular activity could be helpful to drug users; the activity had to be accepted voluntarily by them; it had to be feasible within the context of the Center's staff pattern and the physical setting of Greenwich House.
The last of these requires some clarification. First, the settlement house setting precluded residential treatment and extensive medical care. Second, our activities could not interfere with other Greenwich House activities, many of them used by children. (A subtle form of interference would have been extensive publicity for the Center since it would have created the image of Greenwich House being primarily a center for addicts.) Third, the treatment orientation had to be consistent with the settlement house tradition - benevolent and non-authoritarian.
We initially reviewed all the techniques employed in the outpatient treatment of addicts and decided that the principal activity of the Counseling Center should be the individual counseling of drug users and their families. 7
An important part of the counseling is the referral of patients to appropriate community resources for services which we do not provide, such as public assistance or medical treatment. Other activities are a group work program, group counseling of users and their families, and participation in other Greenwich House activities by selected patients.
Assumptions about the psychological characteristics of drug users
In planning the counseling approach we made certain assumptions about the etiology of addiction and the psychological characteristics of drug users and addicts.
The creation of an addict depends on the availability of drugs in an environment which condones or encourages drug use and an individual predisposition to drug use (6). Regarding the first factor - the control of the availability of drugs - it is primarily a police function. A treatment program may have an indirect effect since reducing the number of drug users reduces the demand for drugs and then their availability. Concerning the second factor, adverse attitudes in families
6This was confirmed by subsequent results (Table I).
7Counseling is a process whereby a patient discusses his problems with a counselor and through a better understanding of himself and through interaction with the counselor is able to modify his behavior. A discussion of the difference between psychotherapy, social casework and counseling is beyond the scope of this paper.
can be modified by counseling. The primary emphasis of a treatment program has to be on the third factor-the predisposition of the individual, or more precisely, the behavior of individual drug users.
Addicts are not a homogenous population but they do have certain common personality or behavioral characteristics. It has been suggested that some of these characteristics exist prior to drug use but become reenforced or accentuated in the course of the drug addiction [ 6] . Among these characteristics are: [ 1] inadequate control of impulses, [ 2] an avoidance of stress and tension, [ 3] an intense desire for immediate and effortless gratifications, [ 4] a disturbance in relationships with authority manifested by either total resistance or submission to external direction and [ 5] persistent exploitative behavior.
Other personality characteristics develop in the course of the drug addiction. Some of these are: [ 1] satisfaction from the use of drugs, [ 2] commitment in varying degree to drug use as a way of life and [ 3] social alienation, especially from non-drug users.
Description of counseling program
The Center is open for counseling Monday through Friday from 9 a.m. to 5.30 p.m. and from 6 through 9 p.m. two evenings per week to accommodate working patients.
New patients either "drop in ", call for an appointment, or have an appointment which was made by the person who referred them. They are first seen by a secretary who fills out an admission sheet and then they are interviewed by a staff member. As we became busier one person was assigned to coordinate intake. He handles the referral calls and schedules the initial appointments, preferably within twenty-four hours, with whoever is available.
We try not to reassign patients after the initial interview because the treatment should begin immediately and all staff members should have an opportunity to treat all types of patients. A small number of cases have to be reassigned to another staff member, usually at the request of the patient.
The counseling follows these general guide lines:
We are non-authoritarian, so as to avoid provoking rebelliousness. The only rules which we emphasize pertain to the treatment process-keeping scheduled appointments at regular intervals.
In view of the addict's inability to delay gratification we avoid extensive initial evaluations and instead focus immediately on current adjustment problems. Also, long initial evaluations are usually a duplication of prior treatment experiences.
We do not provide material services, such as medications and funds, because their availability stimulates addicts' exploitative attitudes and their tendency to make the rules on how these should be provided.
To avoid becoming embroiled in the addicts' rebelliousness we do not emphasize or rely on external coercion to make them participate in treatment. Instead, we express our interest by "reaching out"-calling or visiting them when they miss appointments, or visiting them when they are hospitalized or imprisoned. If they interpret such activity as coercion, we indicate that they always retain the initiative and do not have to see us if they do not want to.
In view of their commitment to drug use we do not pressure them to abstain. We try to help them to understand their drug use and its consequences and remind them that we have no vested interest in their giving up drug use. We encourage them to keep their appointments even when intoxicated.
In view of their crisis-ridden lives and the evidence of inadequate functioning in most areas, we treat all patients intensively. We offer them two appointments per week, lasting from 45-60 minutes. If they miss appointments or come late we make up the time if possible.
Description of patients
Table I lists twenty-five salient background characteristics of the 441 drug users who were seen at the Greenwich House Counseling Center during the first 20 months of operation. They are not strikingly different from groups of adult addicts described by other authors [ 4] , [ 13] , [ 15] .
As was mentioned previously, though we accepted for treatment all drug dependent persons, the vast majority (82.5 %) of our patients used heroin predominantly. Some of those who were using other drugs at the time they came to the Center had used heroin in the past.
Heroin is recognized as the most frequently abused opiate in large urban areas in the United States [ 25] . Our statistics appear to confirm this picture. However, neither of these figures reflects the actual prevalence of the various forms of drug abuse, including nonopiates.
The many reasons for the inaccuracy of the national statistics are discussed by Chein [ 25] . Our own data most probably indicate that persons who use heroin are more apt to seek treatment, possibly because of the high price of the drug, associated social stigma and pressure from family, law enforcement and welfare agencies. Because of its social consequences, heroin use is the most disturbing form of addiction to the addict.
At time of first interview.
|
Arrest history
|
Number of siblings
|
||
|
None
|
16.4 |
Range
|
1-13
|
|
Moderate
|
37.5 |
Mean
|
3.4 |
|
Severe
|
46.7 |
Median
|
2.8 |
|
Years of schooling completed
|
Ordinal position
|
||
|
Range
|
2.5-17 yrs.
|
Only
|
16.0 |
|
Mean
|
10.6 yrs.
|
Oldest
|
27.5 |
|
Median
|
10.9 yrs.
|
Youngest
|
25.9 |
|
Family background
|
Family history of drug abuse
|
||
|
Intact
|
42.3 |
Present
|
18.2 |
|
Slightly disrupted
|
9.3 |
Absent
|
70.3 |
|
Moderately disrupted
|
32.0 |
Alcohol only
|
11.5 |
|
Severely disrupted
|
8.1 | ||
|
Totally disrupted
|
8.3 |
Psychiatric diagnosis
|
|
|
Antisocial reaction
|
16.8 | ||
|
Character trait disorder
|
72.0 | ||
|
Schizophrenic reaction
|
11.2 |
All figures in percentages unlesss otherwise indicated.
Definitions of characteristics in Appendix A.
The number of non-heroin users in our group of patients is too small to affect our overall statistics. A few conclusions about them will be discussed in the second paper.
As is to be expected 90 % of our patients are in Hollingshead's Social Class IV and V [ 9] , meaning that they come from a poor socio-economic environment. Many of the patients in Class II and III were still living at home and were not the heads of their families. Therefore, they were classified on the basis of their families' status rather than their own. Some of them would belong in Class IV or V if they were living alone.
The four-to-one male/female ratio is similar to the figures reported by the Federal Bureau of Narcotics. Also, it parallels sex ratios reported for anti-social activity and alcoholism.
The median age of 29 years closely corresponds to figures for addicts presented by others [ 13] , [ 18] . Ball ( [ 2] has discussed in detail changing age patterns of addicts.
Data on ethnicity and national extraction are particularly important because of their relevance to the socio-cultural factors in addiction and to the frequently made statement that urban addiction is an affliction of minority groups ( [ 5] . The proportion of about one-third Negro and one-sixth Puerto Rican addicts is actually lower than reported by others. Osnos analysed admissions from New York City to the Lexington Hospital and found almost half were Negroes and one-fourth were Puerto Ricans [ 18] . The most likely explan- ation for this difference is that Greenwich Village is a predominantly white neighborhood, 8
The categories in Table I "Italian" and "Irish" refer to second or third generation Italian or Irish Americans. The 14.0% of "Italians" is a reflection of the Greenwich Village neighborhood in which, as mentioned previously, most of the indigenous heroin addiction is amongst Italian-Americans.
Jewish people are of course not an ethnic group, but they have certain common characteristics of family structure and social values. Most of these patients are second or third generation of Eastern-European descent.
Data on religion were not analysed because they are wholly dependent on ethnic and national extraction.
More than half of the patients are single. This is greater than the number of single people in the general population at a comparable age but corresponds to data on alcoholics. The large proportion of patients who are separated and divorced is even more significant since it suggests that those addicts who do marry encounter severe difficulties, either because of their personality problems or the complications of drug use. In a study of the wives of addicts [ 23] , we emphasized the manifold and intolerable problems which exist if one lives with an addict - financial insecurity, danger of arrest and frequent separations. An important but infrequently mentioned hazard of living with an addict is the continuous threat of fire, since many are heavy cigarette smokers and if they are intoxicated they fall asleep and can ignite bedding.
At the time of the first interview at the Center, only 15% of the cases resided in the Greenwich Village neighborhood. Another 22 % came from a ten-block belt bordering this area and the remainder from other parts of New York City. This is probably an indication of low heroin incidence in the neighborhood and does not imply that there is not considerable abuse of other drugs.
Regarding living arrangements, almost half the group live alone. This figure is probably disproportionately high because a quarter of our cases were referred by the Department of Welfare, which places most of its clients who have a history of drug abuse in furnished rooms.
A very high proportion-86%-were unemployed at the time of the first interview. This of course is a measure of their social inadequacy, but the figure may be slightly inflated since many of the patients when first seen at the Center had just been released from a hospital or prison and had not had an opportunity to obtain a job as yet.
The large number and variety of referral sources is a result of our extensive case finding efforts. Also, it shows how many different kinds of agencies come into contact with addicts. The Department of Welfare is the biggest source of referrals (26.5%) because all addicts who seek public assistance are referred as a matter of policy to a treatment service. None of them can decline the referral because they realize this could mean they would not receive public assistance. This policy also affects our figure of 45 % who are receiving public assistance. The proportion of all addicts in New York City who are receiving public assistance is probably much smaller.
Hospitals are the next largest source of referrals. A substantial portion of these came from the Manhattan General Division of Beth Israel Hospital which is a large detoxification center in New York City but does not have an extensive after-care service. Other hospital referrals came from Lexington and from general hospitals where they were treated for associated medical problems.
Prisons occasionally refer drug users who have been involved in treatment while in prison and who desire to continue treatment upon release. Probation Officers also refer many addicts for treatment because they themselves often do not have the time or the skill to handle these difficult cases. Though a probation officer rarely insists that an addict participate in treatment, the implication is that if he does not the refusal will be to his disadvantage.
"Other non-governmental agencies" include social work agencies and specialized programs for addicts. "Other governmental agencies" include schools which are not a frequent source of referrals.
The large percentage of cases referred by other drug users suggests that the program met the needs of those patients who came for treatment and they, therefore, referred their friends.
The three principal reasons for coming to the Center are: ( a) for treatment, ( b) to be referred for detoxification and ( c) to be referred to the Department of Welfare. Undoubtedly a substantial proportion of the 72.9 % of those who said they wanted treatment were primarily interested in satisfying their family, their welfare worker or their probation officer, and had little interest in counseling.
We did not see more patients who wanted to be referred for detoxification because we did not try to get preferential treatment for them and most addicts know where to go directly if they have to be detoxified. The 5.1% who wanted to be referred for public assistance felt it would be easier if they were referred by us rather than going on their own. This group is in addition to the 26.5% who were referred to us by the Department of Welfare and were already receiving public assistance.
Another reason for coming to the Center was to get help with employment. Others came to get a "clean bill of health ". For instance, a former addict who was not using drugs but whose family suspected he was might want us to intercede on his behalf.
Turning to the addiction history and status, less than a third of the patients were using sufficient drugs to be physically dependent at the time of the first interview. Slightly more than a quarter were using drugs but not enough to be physically dependent. A little more that a third were abstinent, but many of these had just been released from a hospital or institution and had not had the time as yet to relapse to drugs. Those who were using non-addicting drugs were using either amphetamines or marijuana. It is to be emphasized that we did not do any physical examinations and the judgments on the degree of drug use depended on the patients' histories and the workers' observations of their physical appearance.
The length of drug use varied from a few months to 53 years with a mean and median of slightly above 10 years, indicating that we were dealing overall with chronic drug users.
The age at the onset of drug use ranged from 10 to 41 years. The median of 18 years indicates that at least half of the patients started using drugs in their adolescence, confirming the findings of other authors [ 4] , [ 5] .
The classic pattern of drug use begins with the smoking of marijuana, turning to intranasal or subcutaneous heroin use and ultimately to intravenous heroin ( [ 5] . In some of our younger patients the initial period of experimentation, prior to heroin use, involved cough syrups, barbiturates and amphetamines instead of marijuana.
In many cases, after the pattern of regular intravenous heroin use is established there is supplementation with barbiturates and glutethimide. Fifteen per cent of the patients admitted to Lexington were physically dependent on barbiturates, in addition to being addicted to an opiate [ 18] .
Marijuana smokers pride themselves on the fact they do not have to turn to heroin since they are satisfied with marijuana. However, we found that most of the users of hallucinogens, such as lysergic acid diethylamide-25 and mescaline, have a history of marijuana smoking. This suggests that some of the marijuana users who are afraid to use heroin because of its legal complications turn instead to the hallucinogens because they want a more intense experience than is provided by marijuana.
There is evidence that as a group our patients have made efforts previously to stop using drugs. They have had, on the average, more than two prior detoxifications. In a third of the cases there was some prior psychiatric or psychological treatment and in another quarter of the cases there was considerable prior treatment.
More than 80% of the cases had a history of arrests. The crimes for which they were arrested are those associated with drug use, such as possession of narcotics or the paraphernalia needed for the use of narcotics; sale of narcotics and various crimes against property. We found that addicts are rarely arrested if they are not currently using drugs. If a patient who is reportedly not using drugs is arrested, usually this indicates that he relapsed to drug use shortly before his arrest.
Turning to the patients' background, half of them completed less than 11 years of schooling. This coincides with their 16th year at which time students are permitted to leave school. Leaving school frequently coincides or shortly precedes the onset of drug use.
There is an extensive literature on the relationship between family disruption and subsequent maladaptive behavior ( [ 20] . More than 50% of our patients came from families which were slightly, moderately or totally disrupted. The most common pattern was the absence of a paternal figure, either by death or separation. The mother, who is expected to fulfill the responsibilities of both father and mother, is unable to do either adequately.
Data on the number of siblings and the ordinal position in relation to other siblings are not significant. The proportion of patients who are either oldest or youngest children is not unusually high.
A positive family history of drug abuse includes parents, spouses and siblings who were using or had used drugs. The frequent occurrence of a family history of alcoholism is probably associated with the low socio-economic status of many of the patients and the frequent family disruption.
Figures on heterosexual and homosexual orientation are indicative of concomitant problems in social relationships and the existence of sexual disturbances. A large proportion (63.9 %) of patients are either promiscuous, totally abstinent or homosexually inclined.
It is generally agreed that drug addiction is almost always associated with severe personality disturbance. Our findings correspond to the views of other authors in that most addicts can be diagnosed most accurately as severe character disorders, usually in the passiveaggressive personality group. [ 4] , [ 5] 5, [ 13] . About a sixth were diagnosed as antisocial reaction (sociopaths or psychopaths) and a little more than 10% were schizophrenic. There is a striking absence of principal diagnoses of psychoneurosis and mental deficiency.
Attendance and attrition
Figures 1 and 2 summarize the attendance patterns during the first two years of the Center's operation. As the Center became known in the community the caseload gradually increased. The total number of patients rose to 90-95 per month and the number of new patients rose to 35-40 per month. The total number of interviews increased correspondingly. However, the ratio of about three interviews per month for each patient did not change.
There was no comparable increase in the number of field visits and the number of relatives interviewed per month. Initially we were very enthusiastic about "reaching out" and made home visits whenever patients did not keep their appointments. We also saw as many relatives as possible early in the course of each patient's treatment. We soon learned that field visits and interviews with relatives could disrupt the treatment if applied indiscriminately. Frequent field visits encouraged dependence and passivity and irritated or frightened many of the patients. Interviews with relatives, early in the treatment, were often misunderstood by the families and by the patients.
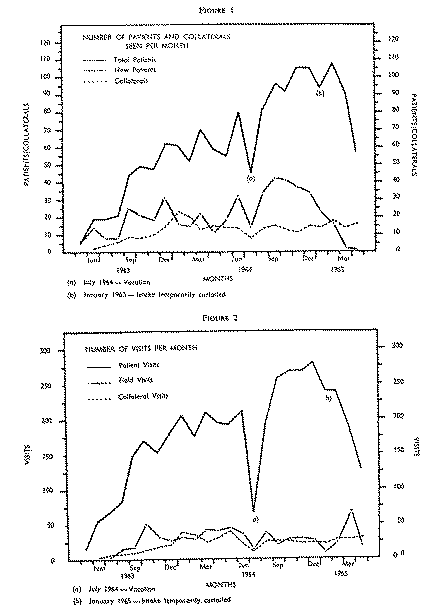
One of the accepted premises regarding the outpatient treatment of drug users is that they do not keep regular appointments [ 4] . We were, consequently, concerned about the possible inefficiency of scheduling regular appointments for our patients. To assess this a record of all scheduled, kept, canceled, broken and late appointments, was maintained. Approximately one-half of the scheduled appointments were kept, one-third were
canceled or broken and one-sixth were late. We thought that as we became more experienced and learned to handle absenteeism and late appointments the proportion of kept appointments would increase. However, this was not the case.
As we anticipated, many patients did not become involved in the counseling: 36% of the patients were seen once; 21% were seen 2-3 times; 16% were seen 4-9 times; 27% were seen ten or more times (up to 100 interviews). These figures seem discouraging at first glance, but actually they are comparable to statistics presented by psychiatric clinics and casework agencies which treat lower socio-economic class patients [ 7] .
The counseling process
Drug addicts' behavior while in a treatment situation has been extensively described by many authors [ 3] (, [ 4] , [ 12] , [ 17] , [ 19] . They are particularly difficult patients because they express their conflicts by "acting out ", instead of talking about them. They relate to people who treat them as they do to others in their lives. They are very demanding in every conceivable way; they expect others to assume responsibility for them; they try to corrupt others; and they play other people against each other for their own gain.
Drug addicts become easily frustrated and flee from any stress. Consequently one of the most discouraging aspects of their treatment is their brittleness. Patients who appear to be doing well encounter some disappointment and almost instantly relapse to drugs. They then appear to lose all power and will to recover, and the staff is left feeling that a great deal of work has been lost.
Our particular approach seems to have two significant effects on their behavior within the treatment situation. First, since we do not force them to participate in treatment we do not have to persuade them that they have problems and conversely they do not have to convince us that they do not have any problems. As a result, they talk more freely about their difficulties and their personal responsibility for what has happened to them. Secondly, since we do not provide any concrete services, such as medication and money, they cannot use the availability of these as a focus for bargaining. Such bargaining frequently becomes another way of avoiding their difficulties.
In summary, in our non-authoritarian setting, where we do not try to lead their lives, either by telling them what to do, or by providing them with services which they could get elsewhere, they are less rebellious and exploitive. Consequently, they are able to examine more freely their own responsibility for their life situation than they did in other settings.
Families of drug users
One of the principal advantages of our neighborhood-based program is its ready accessibility to patients as well as to their families. We were very interested in interviewing the families of our patients so as to understand and to help them. However, our initial enthusiasm in contacting their families occasionally resulted in the disruption of treatment. Certain patients felt that our interest in their families meant that we were not primarily concerned about their personal welfare and that we would side with their families. Others interpreted our request to see their families as proof that the families were entirely at fault and they themselves did not require treatment.
The families similarly misinterpreted our interest. If they already blamed themselves for causing the addiction, they were afraid that we wanted to interview them to hold them accountable. If they had already expelled the patient from the family they were afraid that we would pressure them to take him back. In this connection we found that the addict frequently is emotionally isolated from his family even if he is still living at home. 9This alienation is not entirely attributable to the underlying family dynamics. It is also based on reality-it is extraordinarily difficult to live under the same roof with someone who is using drugs.
If the family denied any responsibility for the addiction they usually wanted rules from us on what to do even though they may have had unsatisfactory results from advice in the past.
One or more collaterals were seen in 28 % of the cases. The probability of a collateral being interviewed increased as the patient's involvement in treatment increased: when the patients were seen only once, a collateral was interviewed in 16% of the cases; if seen 2-3 times, the percentage was 22; if seen 4-9 times, the percentage was 28; it rose to 52% if the patients were seen ten or more times. If no collaterals in the latter group were interviewed, this was usually because the patients had no close relatives or friends.
The principal categories of collaterals interviewed were: mothers 38%; fathers 18%; siblings 11%; spouses 23%; girl friends 5% and others 5%.
One or more relatives received counseling in 12% of the cases. As a matter of policy the relatives were usually treated by a different worker from the one who was working with the patient.
We found that we were unable to treat addicts and their mothers concurrently. Usually when the mother started coming regularly the patient stopped. In contrast,
9At the time of the initial interview, 24% lived with their parents.
concurrent treatment of husbands and wives was moderately successful. In several instances we were able to treat a drug-using husband and his non-drug-using wife for prolonged periods without any unusual problems. The wives, however, usually stopped treatment soon after their husbands stopped. In only one instance we were able to treat a husband and wife, both of whom were drug users.
We organized two groups for counseling of mothers. Both groups met once per week for one and a half hours, one for sixteen sessions and the other for eight sessions. Neither of the groups was successful. The mothers seemed overwhelmed by guilt or else demanded formulas for handling specific situations.
We were unable to involve any fathers or husbands of drug users, confirming the observations of other investigators [ 4] (4).
Group counseling
Two groups for counseling of patients, both led by social workers, were organized during the second year of the Center. The groups met once per week for ninety minutes, one for seventeen sessions and the other for twenty-six sessions.
The erratic attendance in both groups interfered with the development of group cohesiveness. For example, five patients would come to a meeting. The next week none returned and instead three new patients came which, in effect, meant that the worker was starting with a new group. The groups resented new members but at the same time could not accept the responsibility for coming regularly to insure the group's viability.
It is doubful whether the groups had any significant beneficial effect on the patients. Usually those patients who were already involved in and benefiting from individual counseling were more likely to participate regularly in group counseling.
Group work program
The two group workers initially did a detailed survey of the experience of other settlement houses servicing narcotics addicts [ 21] . They found that many settlements in New York City had such experience in the past. They had gradually excluded addicts from their programs because of many problems such as theft and destruction of property. Also, the settlements believed that the addicts were not substantially helped. The survey concluded that a group work program for addicts must be very carefully structured, professionally supervised and tailored to the specific needs of drug addicts.
One of the group workers ran a lounge program for fifteen months. It was designed for hard-core male addicts who lived in the neighborhood and who were known to Greenwich House before the start of the Counseling Center. Most of them were Italian-Americans, as was the group worker. Young male addicts of Italian origin have been considered one of the most disturbed and antisocial subgroups of addicts and particularly resistant to any kind of voluntary treatment intervention.
The group met twice a week from 7 p.m. to 10 p.m. in a sitting room which was separated from other Greenwich House programs. The principal activity was the preparation of a meal. The patients decided on the menu (usually Italian food of the type they were served at home). The worker purchased the food and the group cooked the meal. After the meal they participated in sedentary activities, such as playing poker for cigarettes. During the summer the group went on several excursions-to the World's Fair, movies, amusement parks and to the beach.
The worker encouraged them to follow simple ground rules which were, for them, none the less difficult. For example, they were expected to help in the preparation of the meal and in cleaning up, and they were not supposed to start eating until the meal was ready. They were permitted to come to the lounge if intoxicated, but it was agreed that they were not to take drugs on the premises of the settlement house.
Seventeen patients participated in this group; six came regularly, six periodically and five on occasion. Of the latter, three were Jewish. Although they knew the other patients, they came rarely because they were no more than tolerated by the others.
The group was successful in several important ways. Though participation was entirely voluntary, one-third attended regularly and were positively disposed toward the program. Unfortunately all of them had frequent periods of incarceration or hospitalization so that at times many members of the group were not available.
The worker was able to keep significant acting-out to a minimum without becoming authoritarian. For example, if he observed that a member went to the bathroom apparently to take drugs (heroin, cough syrup or assorted pills), he only had to indicate to him that he was aware of what was going on and even though the man rarely admitted to having taken drugs he would not do it again for several sessions.
The worker had an unparalleled opportunity to study the behavior of a group of deeply disturbed individuals who were actively using drugs. He frequently observed that heroin had a regressive effect on them.
They were more demanding, they were guilessly testing him, they obtained obvious gratification from daydreaming and their interaction was similar to the "parallel play" of small children.
On the debit side, it appeared that this kind of limited program had minimal impact on the participants' overall adjustment. The amount of responsibility which they voluntarily accepted was minimal. We felt that if the program were rapidly expanded either by meeting more frequently or introducing more demanding activities, many of them would have stopped coming either because the stress was too great or because the program was interfering with their drug use.
In summary, this program demonstrated that this particular group of addicts does not use drugs merely to prevent abstinence, but also to become as intoxicated as possible. While they are in such a state, they are capable of only minimal functioning. It is unlikely that this experience with collaborative activity carried over to other areas of social functioning.
We described the other Greenwich House activities such as the Adult Education Classes and the Music School to most of out patients to find out if they wanted to participate. Only a small number expressed an interest in these activities, and almost all of those did not participate consistently enough to obtain any tangible benefit.
Community relationships
Because of the many complex social, legal and medical ramifications of drug addiction and the constant public attention which is focused on this problem, it was essential to communicate and work with many other agencies. We have already mentioned our efforts with regard to case finding. The staff also participated in frequent lectures and panels on addiction which were conducted for professional and non-professional groups such as school physicians and social workers, Department of Welfare workers and various neighborhood groups. We participated in mass media programs through radio and television appearances and interviews with newspaper writers.
There were numerous visitors to the Center. These included various professional trainees who wanted to learn about addiction and the staff of other agencies who were working with addicts. Additionally, there were 22 conferences with professionals who came to us because they were planning to start treatment programs for addicts.
Other community activities included: answering written and telephone requests for information about drug addiction and the Center; telephone consultations regarding addicts who were unknown to the Center; consultation pertaining to cases on which we collaborated with other agencies.
Our expeditious intake procedure was in a sense a community activity since it provided a valuable service for agencies which did not treat or provide services for addicts. By readily accepting the referral of a troublesome patient we freed these agencies to use their time for other services.
Collaboration with Departments of Welfare and Probation on patients for whom we were jointly responsible was extremely important. These are large organizations with many experienced, but not professionally trained, workers, which have a dual responsibility to their clients as well as society. Because of addicts' tendency to play persons in authority against each other, we planned each aspect of the collaboration. For instance, we told patients in advance how much information we would share with their probation officers or welfare workers. Usually, we only told these workers whether the patients were keeping their appointments. We were particularly reluctant to give them advice on how to manage these patients because we felt that they had their own regulations with which we were frequently unacquainted. Also, we did not want the patients to feel that we were indirectly controlling their lives by influencing their probation or welfare workers.
Conclusions and summary
The Greenwich House Counseling Center was started in 1963 to fill a void in the existing treatment services for drug addicts-a professionally staffed community-based counseling service operating in a non-governmental setting.
The principal treatment modality is the individual counseling of drug users and their families which is tailored to their specific needs. A simplified intake procedure and the elimination of extensive initial evaluations permit prompt involvement in the addicts' current problems. The attitude of the staff is non-authoritarian, with no pressure placed on patients to abstain from drug use or to seek employment. They are encouraged to keep regular appointments even when intoxicated.
Other services include group therapy of patients and families, a limited group work program and referrals to appropriate agencies for medical and financial assistance.
A large number of drug users, referred by many sources, have sought treatment at the Center. More than 80 % of them use heroin predominantly. Others use marijuana, amphetamines, barbiturates, glutethimide and various hallucinogens. Most of the patients are
chronic users who are deeply involved in drug use and associated activities. They have characteristics of addicts described by others: a low socio-economic status, disrupted family background, evidence of inadequate social and vocational functioning and disturbed personalities. They have been arrested frequently and have tried to stop using drugs many times previously.
The minority who are less involved in drug use are socially and psychologically a more heterogeneous group.
Our principal task is getting them committed to a treatment experience so that we can have an impact on their lives. The attrition rate is high-57% are seen three or less times. When they do come regularly, treatment is interrupted by frequent hospitalizations and incarcerations. On the positive side, they seem more willing to discuss their problems with us than in a hospital or other settings where there is an element of authority.
A vital and practical conclusion from the Center's experience was that it is possible to operate a treatment service for addicts in the same physical setting where there are non-addict clients. During the two years, our patients were only occasionally disruptive and their presence did not interfere with the other programs of the settlement house, including those for children and adolescents.
APPENDIX A
Definitions of group characteristics and treatment variables
Age. To nearest birthdate.
Ethnicity. Based on father's ethnic origin.
Area of Residence (Reference to New York City only)
Village. Below 14 Street and West of Broadway.
Periphery. Manhattan-below 28 Street.
Elsewhere. Other neighborhoods.
Reasons for Coming
Treatment. Counseling or psychotherapy.
Detoxification. Referral to a hospital for withdrawal.
Department of Welfare. Referral for public assistance.
Amount of Drug Use. Determination made solely from patient's account of his drug use-no confirmation or laboratory tests. Addicted. Physically dependent.
Not addicted. Not using enough of addictive substances to be physically dependent.
Abstinent. For at least one week prior interview.
Using a non-addicting drug-e.g., marijuana, amphetamines.
Age at Onset. With respect to consumption of all drugs except alcohol.
Length of Drug Use. Total time from age of onset to present-periods of incarceration and voluntary abstinence are not subtracted.
Prior Treatment. Include psychotherapy, counseling and other psychological modalities (e.g., hospital rehabilitation). Minimal. Less than three contacts. Considerable. Four or more contacts.
Number of Detoxifications. Withdrawal in hospital setting only.
Arrest History
Moderate. Less than four misdemeanor arrests.
Severe. Four or more misdemeanor arrests or one or more felony arrests.
Family Background
Intact. 2 stable parental figures.
Slightly disrupted. 2 slightly unstable parental figures. Moderately disrupted. 1 stable or 2 unstable parental figures. Severely disrupted. 1 unstable parental figure. Totally disrupted. No parental figures.
Psychiatric Diagnoses. All diagnoses made by director, either through direct interview or after discussion with worker.
8Chein [ 5] found the prevalence of narcotic addiction varies widely in New York City depending on the specific neighborhood studied. It is highest in deprived areas where there are large Negro and Puerto Rican populations. Greenwich Village is not one of the high prevalence addiction neighborhoods of New York City.
In the 1960 Census, 8% of the New York City population was Puerto Rican and 14% was Negro.
Alksne, H., et al., Follow-up study of treated adolescent users, Columbia University School of Public Health and Administrative Medicine, N.Y., 1959.
02Ball, J. C., Two Patterns of Narcotic Drug Addiction in the United States, J. of Criminal Law, Criminology and Police Science, 56, No. 2, 1965, 203-211.
03Boshes, B., et al., Management of the Narcotic Addict in an Outpatient Clinic, American J. Psychiatry, 113, 1956, 158-62.
04Brill, L., et al., Rehabilitation in Drug Addiction , Mental Health Monograph 3. U.S. Department of Health, Education and Welfare, May, 1963.
05Chein, I., et al., The Road to H , Basic Books, Inc., N.Y., 1964.
06Council on Mental Health, AMA and Committee on Drug Addiction and Narcotics, The National Academy of Sciences-National Research Council, A Statement on the Use of Narcotic Drugs in Medical Practice and the Management of Narcotic Addicts, Spring, 1963.
07Goin, Marcia Kraft, et al., Therapy Congruent with Class Linked Expectations, Arch. Gen. Psychiatry, 13, 1965, 133-137.
08Hansberry, Lorraine, A Sign in Sidney Brunstein's Window, Random House, N.Y., 1965.
09Hollingshead, A B Two-Factor Index of Social Position, New Haven, Conn., Author, 1957.
10Jaffe, J. H., Drug Addiction and Drug Abuse, in Pharmacological Basis of Therapeutics, Eds. Goodman & Gillman, McMillan, N.Y., 1965.
11Kerouac, Jack, On the Road, the Viking Press, N.Y., 1955.
12Laskowitz, D. & Osnos, R., Treatment of the Drug Addict on an Outpatient Basis, Clinical Med., 72 , 1965, 325-331.
13Lowry, J. V., Hospital Treatment of the Narcotic Addict, Federal Probation Quarterly, 20, No. 4., 1965, 42-47.
14Mason, P., Observations on Hospitalized Adolescent Drug Addicts, N.Y. State J. of Med., 57, 1957, p. 67.
15Narcotic Drug Addiction, Mental Health Monograph , No. 2, U.S. Department of Health, Education and Welfare, P.H.S., 1963.
16Nyswander, Marie, et al., The Treatment of Drug Addicts as Voluntary Outpatients: A Progress Report., American J. Orthopsychiatry, 28, 1958, 714-727.
17Osberg, J. W. & Lewis, J. M., Observations on Institutional Treatment of Character Disorders, American J. Orthopsychiatry, 28, 1958, 730-744.
18Osnos, R., Drug Addiction in Women, unpublished paper, 1961
19Osnos, R., The Treatment of Narcotics Addiction, N.Y. State J. Med., 63, 1963, 1182-8.
20Pitts, F. N., et al., Adult Psychiatric Illness Assessed for Childhood Parental Loss, and Psychiatric Illness in Family Members - A Study of 748 Patients and 250 Controls, American J. Psychiatry, 121, 1965, Supp.
21Quartaro, P. & Pierson, A., A Survey of Settlement HouseExperience with Narcotics Addicts, unpublished paper, 1964.
22Raskin, H. A., A Proposed Community Project for Rehabilitation of Narcotic Addicts, Digest of Paper, American J. Orthopsychiatry, 34, 1963, 396-397.
23Taylor, Susan, et al., The Wives of Drug Addicts, Paper presented at Annual Meeting of American Psychiatric Association, May 1965.
24What's New, Abbott Laboratories, 220, The Public Health Service Narcotics Hospital at Lexington.
25White House Conference on Narcotic and Drug Abuse, U.S. Government Printing Office, Washington 25, D.C., 1962.