Laboratory procedures
Experimental
Barbiturates
Narcotics
Amphetamines
Discussion
Acknowledgement
Author: D. J. BERRY , J. GROVE, B. WIDDOP , J. H. P. WILLIS
Pages: 31 to 37
Creation Date: 1970/01/01
The treatment of drug dependence is notoriously difficult. There are few topics in medicine which have aroused such strong feelings, elicited so many biased attitudes or attracted the same amount Of general and often misinformed publicity. To Freedman [1] we are indebted for enunciating five basic principles, one of which deserves emphasis in the present context, viz. "Total abstinence as the primary treatment goal for every patient is unrealistic - a variety of treatment goals are available and each patient should be studied so that a rational treatment plan can be devised in each case."
With the opiates, treatment failures are so common that the question arises why total abstention as the primary objective is so highly prized. So many factors enter into the aetiology of drug dependence that it is conceivable that the addict might be rehabilitated as a reasonable member of society while continuing to take at least a modicum of his drug. This does not mean that opiates should be routinely prescribed to those demanding them for, as Chein [2] , [3] has shown, the requirements vary enormously. Besides being justified in some instances to alleviate withdrawal distress, the discriminating provision of narcotic drugs for dependent patients may be a valuable manoeuvre at the same time as the measures of rehabilitation are being organised and applied.
With heroin (diamorphine) the exercise of continuing the drug is a delicate one, for the user is rarely " straight ", but either " sick ", or " high " [4] i.e. veering rapidly from one extreme to the other. Nevertheless, following the recent changes in legislation in the United Kingdom[5] and the establishment of treatment centres for out-patients, the repeated prescription of heroin is a practice which is currently-being carefully evaluated. While total abstention may be the ultimate aim, heroin is still offered to those patients who, after careful appraisal, are regarded as being unmanageable, for the time being at least, if the drug is totally withdrawn. These patients then attend regularly for examination, interview, guidance, assistance in various ways and follow-up, while they collect their drugs in authorised quantities from retail pharmacists to whom the prescriptions, issued by the doctors in the treatment centres, have been sent separately by post.
The best way of arriving at a suitable dose is to admit the patient to hospital for at least 24 hours and then to find out, under controlled conditions, what is the minimum amount of heroin that is needed for
" stabilisation ". To this arrangement, few of the addicts are agreeable. Instead, therefore, the clinician must rely on inspired guesswork, backed up by other evidence, e.g. the visible numerous injection sites, needle tracks, etc. From the outset, however, it is essential to know whether the patient is in fact on the drug at all, for the supplicants' claims, pleas and protestations are seldom reliable. Subsequently, it is important to check that the drug prescribed and that alone is being taken. For this purpose, known bona fide samples of urine may be tested in the laboratory, but the methods employed for examining them must be rapid, simple, cheap and, above all, reliable. Not, perhaps, that the same, absolute accuracy is demanded in these clinics as in New York [6] , where legal action and conviction may be dictated by the findings. Nevertheless, the validity of the laboratory results must be such as to discover what each patient is taking and to check his or her claim - in other words, to counter assertions with objective evidence. This report describes recent experience in the Guy's/ King's College Hospital Drug Dependence Unit where urine screening has been in use since May, 1968.
Of the total of 147 new patients seen at this Unit from the time it opened in November, 1967, approximately 100 now attend regularly. Examination of their case records revealed findings similar to those described elsewhere [7,8,9,10] . Most of the patients were under 21 years of age, with family backgrounds notable for parental separation and divorce, alcoholic excess and psychiatric disorder. There was also a high incidence of persistent truancy (80 %) and delinquent behaviour antedating drug misuse (51 %). Work records were poor and, in general, the circumstances of the subjects confirmed the expectation of considerable psychiatric and social pathology. Not surprisingly these patients often misrepresent the amounts of drug they take in the hope that will get more than they need, either to ensure that they will always have a reserve or else in order to sell the surplus. Hence it is an advantage to have some laboratory test which will not only ascertain the particular drug being administered but also afford some means of detecting how much of it is being used at a time. Unfortunately this stage of technical advance has not yet been attained.
Obtaining blood for examination, except with a fully co-operative and voluntary patient, raises the problem of " assault ". Urine is much more convenient, both practically and ethically. Mannering et al. (11) were responsible for valuable work initially. They extracted alkaloid drugs from urine into chloroform and carried out the subsequent separation and detection by paper-partition chromatography. This technique has served as a principle upon which a variety of modifications has since been devised for routine analysis. Thus, a preliminary hydrolysis to release the conjugated bases leads to an increase in sensitivity. Then, by performing two alkaline extractions, one at pH 11 with chloroform and a second at pH 8-9 with chloroform/ethanol (9:1), the codeine and papaverine are separated on the one hand from the morphine on the other.
The time limitations imposed by paper-chromatography led to this technique being superseded by thin-layer and gas-liquid chromatography. Cochin and Daly [12] demonstrated that a variety of analgesic drugs could be separated on thin-layer plates. Their extraction procedure differed slightly from that of Mannering, ethylene chloride being preferred to chloroform. As detection reagents they chose iodoplatinate or Dragendorff's solution.
Davidow et al.[13] attempted to overcome the need for two-dimensional chromatography and the use of several developing solvents by introducing a solvent system capable of giving a much better separation of morphine from other narcotics. This consisted of ethyl acetate, 170 ml: methanol, 20 ml with conc. ammonia, 10 ml, and this was used in conjunction with a series of reagents, including iodoplatinate and Dragendorff's, sprayed serially on to the plate. These workers considered that the sensitivity of the method obviated the need for preliminary hydrolysis of the urine.
Parker and Hine [14] developed a highly detailed procedure based on the Cochin-Daly method. They applied two different treatments to the urine sample and termed these Test A and Test B respectively. Test A included an acid hydrolysis step in which the urine was acidified with concentrated hydrochloric acid and heated for 30 minutes at 120o C. After making extremely alkaline with 16 N potassium hydroxide, the mixture was extracted with n-butanol. Back-extraction with 1 N sulphuric acid was followed by re-extraction into 10 % ethanol/chloroform at pH 8.6. The organic phase was taken to dryness and redissolved in a small amount of acetone/methanol solution and fractionated by T.L.C. in ethanol: conc. NH 3:l,4 dioxan: benzene (10:11: 80:100), spots being located by spraying with Dragendorff's and the iodoplatinate reagents. Test A identified those narcotic substances not destroyed by acid hydrolysis which included morphine, codeine, nalorphine oxycodone, hydromorphone, metopon and hydrocodone.
For Test B, a second urine aliquot was adjusted to pH 10, sodium chloride was added and the mixture extracted twice with chloroform. After washing the pooled chloroform extracts with a weak ammonia solution, two back-extractions with 1 N sulphuric acid were carried out and the combined acid fractions made alkaline (pH 10). Sodium chloride was again added and this fraction was extracted twice with chloroform. One drop of 0.5 % sulphuric acid was added to the pooled and filtered chloroform extracts which were then taken to dryness. The redissolved residue was fractionated by T.L.C. in an ammoniacal methanol solvent (3:200) and detected by Dragendorff's and iodoplatinate reagents.
Test B detected methadone, pethidine, cocaine, amphetamine, methylamphetamine, cyclazocine and D-propoxyphene. Although this procedure provides for good specificity over a wide range of narcotics and other drugs of abuse, the diversity of manipulations make it unattractive as a routine method.
A novel modification by Dole et al. (15) dispensed with solvent extraction in favour of absorption of the drugs on cation-exchange paper, with subsequent elution using a series of two-phase buffer solutions, the object being to overcome difficulties presented in the transport of liquid samples for analysis. After concentration of aliquots of the organic phases, thin-layer chromatography in ethyl acetate, methanol and concentrated ammonia (85:10:5) was carried out. Better resolution of the barbiturate fraction was obtained by using a chloroform/acetone (9:1) running solvent. This group of substances was detected by spraying with 0.5 % sulphuric acid followed by 1 % silver acetate and irradiation with ultraviolet light. To detect the alkaloid components a series of sprays was applied successively to the plate. These were 0.5 % sulphuric acid, iodoplatinate reagent, ammoniacal silver nitrate or Marquis reagent and finally, 0.02 M permanganate solution. The ammoniacal silver nitrate and Marquis reagents were given as specific tests for the presence of morphine. Dole recommended ninhydrin as a detection reagent for amphetamines; but experience has shown this to be an extremely non-specific and unreliable test for this group of compounds. Enzymatic hydrolysis of narcotic conjugates was suggested to increase the sensitivity, but this was not incorporated into the routine procedure. Again, the method is lengthy and somewhat involved; furthermore, one would not expect the anionic barbiturates to be taken up by the cation-exchange resin (16). The fact that small amounts of barbiturates are taken out of the urine may be explained by the absorption of this group of drugs on to the cellulose of the supporting paper, in which case rather low recoveries of these could be expected. Mule (16) examined the sensitivity of this procedure using labelled drugs and obtained recoveries of 21.7 ± 5 %, 2.4 ± 0.8 % and 2.1 ± 1% for morphine, pentobarbitone and amphetamine respectively. He concluded that the method was unacceptable for detecting barbiturates, amphetamines or phenothiazines.
Marks and Fry [17] in their paper on their detection and identification of amphetamine and morphine in urine, used a slight modification of Dole's method. An acidic extraction with ether was followed by a second ether extraction at high pH. This extract, designed to remove amphetamines, was then dried with anhydrous sodium sulphate, a procedure which in our experience can cause losses of up to 90 % of amphetamine due to absorption on the salt. Thinlayer chromatography on the concentrated extract followed, with detection by the sensitive Fast Blue B reagent. In view of their drying and evaporation procedures, a gross loss in sensitivity was to be expected; they state, however, that for definitive identification of amphetamine and its congeners further confirmation by gas-liquid chromatography is essential, since the metabolites of amitriptyline, nortriptyline and imipramine have similar chromatographic and tinctorial properties on T.L.C. For narcotic detection, the procedure became more complex, following basically the technique of Dole [15] , in which the drugs were taken on to a cation-exchange resin and eluted with two-phase buffer solutions. Their running solvent for the subsequent T.L.C. consisted of ethyl acetate: methanol: concentrated ammonium hydroxide (170:20:10) and iodoplatinate was used as a spray reagent. As a confirmatory test for morphine, the latter was eluted from the plate, converted to pseudomorphine and its fluorometric emission and activation spectrum determined. (We have been unable to reproduce this last step in the procedure, which itself suffers from the same criticisms of time consumption and complexity as that of Dole.)
Cochin [18] attempted direct thin-layer chromatography of samples by streaking hydrolysed urine on the plate. After development and detection with iodoplatinate, the alkaloid bands were eluted off and rechromatographed in a series of running solvents. He also reported that alkaloid glucuronides spotted on thin-layer plates coated with silica gel-G, prepared with 6 N hydrochloric acid, were hydrolysed on the plate when heated at 150o. The amount of free morphine, and thus the sensitivity, was said to be increased fourfold by this procedure. The technique was said to be applicable also to the detection of barbiturates in urine. It is claimed that as little as 2.5 &mug of morphine is detectable in 100 ml of urine by this procedure.
In practice, the spotting and developing of thinlayer plates is more time-consuming than carrying out solvent extraction and it would seem, therefore, that the suggested direct manipulation can only lengthen such investigations.
Even this brief resume of some of the more important contributions to the field reveals that opinions vary widely on several procedural aspects. Our own procedure, which follows, is yet another modification but wherever possible the technique has been kept short and simple without excessive sacrifice of specificity or sensitivity.
Reagents
All solvents are analytical grade, as are the chemicals used to prepare the spray reagents.
Spray reagents:
Mercurous nitrate:
1 % aqueous solution.
F.P.N.:
5 % ferric chloride solution, 20 % perchloric acid,
50 % nitric acid; mixed in the proportions 1:9:10;
Trinder's reagent:
40 g. mercuric chloride dissolved in 850 ml. of water with warming. Cool, add 120 ml. of N HC1 and 40 g. Fe(NO 3) 3.9H 2O and make up to 1 litre with water.
Iodoplatinate reagent:
3 ml. 10% aqueous platinum chloride, 97 ml. water, 100 ml. 6 % aqueous KI. (Stored in brown bottles.)
Preparation of thin-layer plates
Glass-plates (20 x 20 cm.) are coated with a 250-g layer of silica gel-G prepared from a 30 g/60 ml slurry. These are allowed to dry for 15 minutes, heated for 30 minutes at 100o C and stored in a dessicator.
Spotting of plates
Prior to development, a series of parallel lines 1 cm apart are constructed using a "comb" device (19) thus forming a series of parallel columns for concurrent analyses of several samples. Extracts are applied with a micro-pipette.
Procedure
About 50 ml of urine are collected from each patient with suitable precautions for sample identity. Three bottles fitted with polythene caps are then each half-filled with urine (approx. 10 ml). One bottle is used to examine for barbiturates, the second for amphetamines and the third for narcotics. The remainder of the specimen is reserved to check for the presence of other drugs, e.g. salicylates and phenothiazines.
To one bottle is added 1 ml of N HCl. After checking that the pH is approximately 2 (Universal Indicator Paper), the bottle is filled with chloroform.
Vigorous shaking is applied for 5 minutes (Griffin flask-shaker) and centrifugation at 3,000 rpm for 5 minutes.
The upper, aqueous phase is removed and the chloroform layer filtered through Whatman No. 90 paper.
The organic phase is evaporated to dryness in a conical centrifuge tube at 60o C under a stream of air and the residue taken up in 0.1 ml of ethanol dried over sodium sulphate.
30 &mul are applied to a thin-layer plate along with 10 &mul each of standard solutions (1 mg/ml) of barbitone, phenobarbitone and amylobarbitone.

Running Solvent - Chloroform: acetone (9:1); Spray Reagent - Mercurous nitrate; Columns 1-3 - Barbiturate standards; Column 4 - Blank urine extract from a normal subject; Columns 5-7 - Positive urine extracts from barbiturate addicts; Column 8 - Blank urine extract from a subject addicted to other drugs.
The plate is run in chloroform/acetone (9:1) for 10-14 cm, air-dried and sprayed with 1% mercurous nitrate solution. Barbiturates and their metabolites appear as black or white spots on a grey background.
The urine in the second bottle is saturated with sodium bicarbonate to bring the pH to 8.5; and the bottle is filled with chloroform/isopropanol (9:1).
Vigorous shaking is carried out for 10 minutes, followed by centrifuging at 3,000 rpm for 5 minutes. Any emulsions may be removed by discarding the aqueous phase, adding a further 5 ml of chloroform, shaking manually for a few seconds and re-centrifuging.
The clear organic phase is filtered and taken to dryness as before, the residue being re-dissolved in 0.1 ml of dried ethanol.
30 &mul of this extract are applied to separate sections of a T.L.C. plate. One section has 10 &mul standard solutions (1 mg/ml) of morphine, codeine and methadone applied to it; the other, 10 &mul of a standard solution of chlorpromazine (1 mg/ml).
The plate is developed in ethanol: concentrated ammonium hydroxide:l,4 dioxan:benzene (5:5:40:50) (14) for 10-14 cm and air dried, care being taken to remove all the ammonia since this can lessen the sensitivity of the detection reagents. The phenothiazine section is sprayed with F.P.N. and the narcotic section with iodoplatinate reagent. The narcotics appear as blue and purple spots of varying intensity; since several phenothiazine metabolites will also react with this reagent, a concurrent test as indicated helps to eliminate possible anomalous results.
After spraying, the plate is stood in a tank containing a beaker of concentrated ammonium hydroxide until the spots fade. This converts morphine to pseudomorphine which can be seen as a fluorescent spot under ultra-violet light (254 m&mu).
Although cocaine and methadone give different colours with the iodoplatinate reagent, this solvent system does not separate these drugs. As a distinguishing test, a second plate is run in methanol:12 N ammonium hydroxide (200:3) carrying the sample and standards of cocaine and methadone.
To the third bottle of urine, 1 ml of 2 N sodium hydroxide is added and this is checked for pH 9-10 (Universal Indicator Paper).
The bottle is filled with ether and vigorous shaking carried out for 10 minutes followed by centrifugation at 3,000 rpm for 5 minutes.
Evaporation is then performed in a conical test-tube at room temperature under a stream of nitrogen to approximately 100 &mul. This extract must not be taken to dryness since all the amphetamine would then be volatilised. Further, evaporated extracts must be stored at - 5o C if they are not to be analysed immediately (20).
Five &mul of this material are injected into a gaschromatograph and fractionated on a 5-foot column containing 10 % Apiezon L plus 10 % KOH on 80/100 AW/DMCS Chromosorb W, with a nitrogen flow-rate of 55 ml/min and an oven temperature of 140o C, having first ascertained the retention times of standard solutions of amphetamine and methylamphetamine.
Spot-tests for salicylates and phenothiazines
To 1 ml of urine is added 1 ml of Trinder's reagent: a violet colour indicates the presence of salicylates.
To 1 ml of urine is added 1 ml of F.P.N., when a red colour may indicate phenothiazines. Large amounts of phenothiazine drugs are required for a definite positive result with this test, the T.L.C. procedure already described being much more sensitive.
Opinions differ as to the need for pre-hydrolysis of urine samples. Acid hydrolysis would appear to be a reasonable way of achieving greater sensitivity for the conjugated narcotics. That such a drastic measure could result in destruction of more labile drug components and lead to the formation of misleading byproducts is, however, a distinct possibility. The gentle and specific enzymic incubation method using &beta-glucuronidase is more commendable, but lengthy and rather prohibitive in cost. In our experience, any pre-hydrolysis treatment is quite unnecessary for the majority of samples encountered.
The chloroform/isopropanol solvent was found to be the most efficient extractant, but there is little to choose between this and others recommended in the literature. Experience suggests that the developing solvents of Parker and Hine [14] give the best separation of morphine and codeine, two commonly occurring drugs, although the existence of data on the behaviour of narcotic drugs in so many other systems has proved invaluable in cases where further confirmation has been required.
Little disagreement as to the choice of spray reagents is to be found, iodoplatinate being very satisfactory for the detection of the narcotics. It is essential, however, that some confirmatory test for morphine be carried out.
Several authors claim specific detection of amphetamines on T.L.C.; it is our experience and that of Marks and Fry[17] that these results, especially where such non-specific spray reagents as ninhydrin are used, are extremely unreliable due to interference from other drugs and their metabolites, notably from the triptyline, imipramine and phenothiazine groups. It would appear essential to confirm any such findings by gas-chromatography; indeed, several workers [21] [22] have demonstrated the possible applicability of this technique to the complete screening of urines.
Using the procedure we have described, it is possible for two junior technicians to screen 15-20 urine samples in a working day of 8 hours. Considerable experience is often required, however, in interpreting the results, since the appearance of extraneous spots on the chromatogram is a frequent occurrence. These may indicate an uncommon drug, metabolites or very often the presence of nicotine and its metabolites in the urine of a heavy smoker. It is recommended that a control urine sample taken from a smoker should be examined in order that these characteristic spots can be readily recognised. For instance in figure 4, column 4, three "smoker spots" are seen with approximate Rf values of 0.2, 0.4 and 0.8. It is apparent that these could interfere with the detection of codeine (column 5) and morphine (column 7). Further, in figure 5, the three" smoker spots" are now running together with an approximate Rf value of 0.7 (columns 3 and 4) and thus may confuse the detection of cocaine. As is to be expected, the heavier the smoker, the greater the difficulties in interpretation encountered.
In order to establish the limits of detection of the procedure with respect to time after ingestion of the drug, known quantities were administered orally to normal volunteers. These subjects collected their urine at intervals and samples were taken through the test as previously described. The following results were obtained:
| Drug | Dose | Detectable after |
|---|---|---|
Morphine
| 10 mg.
| 5 hours |
Codeine
| 8 mg.
| 14 hours |
Methadone
| 10 mg.
| 24 hours |
Amphetamine
| 10 mg.
| 48 hours |
Cocaine
| 10 mg.
| Not detectable
|
after 2 hours
|
Clearly, the higher dosage r?gime of the addict will bring his urinary drug levels well within the range of sensitivity of the procedure.
Application and results of urinary screening in addicts
Ten patients who claimed to be injecting themselves with heroin were found to have urines negative for morphine. When challenged, they denied the validity of the findings but repeat examinations failed to demonstrate the presence of morphine, although other drugs were found in their urine with the exception of one patient whose urine remained drug free.
Bk - Blank urine extract
| Cp - Chlorpromazine
| Ph - Pheuothiazines
|
Cc - Cocaine
| Me - Methadone
| NS - Non-smoker
|
Cd - Codeine
| Mo - Morphine
| S - Smoker
|
![Full size image: 6 kB, Running Solvent - Ethanol: concentrated sodium hydroxide: 1,4 dioxan: benzene (5:5:40:50): Spray Reagent - Iodoplatinate; Columns 1-2 - Narcotic standards: Columns 3-6 - Positive urine extracts[...]](/images/bulletin/bulletin_1970-01-01_3_page005_img002_small.gif)
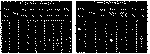
Eleven patients who claimed to be injecting themselves with methylamphetamine and taking drinamyl tablets showed negative urines. This was an interesting finding since these were all patients who came to the clinic demanding prescriptions of methylamphetamine during an epidemic of methylamphetamine abuse in London. At least six of these patients had been taking tablets intermittently but their claims of regular self-injection were false.
Finally there were two patients who showed the presence of unexpected substances in their urine. One was a middle-aged alcoholic who showed dromoran in his urine on one occasion, the other was a young woman in her twenties - referred for investigation of alcohol and possible drug abuse. Morphine was found in her urine, though its use was denied. Unfortunately she never returned to the clinic for subsequent assessment.
Further experience with urinary screening provides the clinician with the value of a procedure which is simple, reliable, cheap and acceptable to the patient. It provides a satisfactory way of random checking on patients receiving drugs on prescription.
The co-authors wish to thank Dr. Roy Goulding for encouragement and considerable guidance in the preparation of the paper and Miss J. Hiscock for invaluable technical assistance.
A. M. Freedman, "Towards a rational approach to the treatment of Narcotic Addictions: Basic Notions" in " Addictive States ", edited by A. Wikler, Res. Publ. Ass. Nerv. Ment. Dis ., XLVI, XXX, 378-386 (1968).
002I. Chein, D. L. Gerard, R. S. Lee and E. Rosenfeld, "Narcotics Delinquency and Social Policy - The road to H" (1964), published by Basic Books, New York.
003I. Chein, " Narcotics ", edited by D. M. Wilner and G. G. Kassebaum (1967), published by McGraw-Hill.
004V. Dole and M. Nyswander, Arch. Intern. Med., 118 , 304 (1966).
005Dangerous Drugs (Supply to Addicts) Regulations 1968.
006M. Oho, B. F. Engelke and C. Fulton, U.N. Bulletin on Narcotics , XXI, 31 (1969).
007T. H. Bewley, U.N. Bulletin on Narcotics , XVIII, 1 (1966).
008T. H. Bewley, O. Ben-Arie and I. P. James, Brit. Med. J., I , 725 (1968).
009J. H. Willis, "The Natural History of Drug Dependence" to be published in Symposium on Scientific Aspects of Drug Dependence (1969).
010J. H. Willis, "U.K. and U.S. Addicts - Demographic and Psychiatric Aspects" to be published in Brit. J. Addict. (1969).
011G. J. Mannering, A. C. Dixon, N. U. Carrol and D. B. Cope, J. Lab. Clin. Med., 44 , 292 (1954).
012J. Cochin and J. W. Daly, Experientia, 18 , 294 (1962).
013B. Davidow, N. Li Petri, B. Quame, B. Searle, E. Fastlich and J. Savitzky, Am. J. Clin. Path., 46 , 58 (1966).
014K. D. Parker and C. H. Hine, U.N. Bulletin on Narcotics , XIX, 51 (1967).
015V. P. Dole, Wan Kyun Kim and I. Eglitis, J.A.M.A., 198 , 115 (1966).
016S. J. Mule, J. Chromatog., 39 , 302 (1969).
017V. Marks and D. Fry, Proc. Assoc. clin. Biochem., 5 , 95 (1968).
018J. Cochin, Psychopharm. Bull., 3 , 53 (1966).
019I. Sunshine, private communication, Poison Information Center, Academy of Medicine, Cleveland, Ohio (1968).
020D. B. Campbell, J. Pharm. Pharmac., 21 , 129 (1969).
021K. D. Parker, C. R. Fontan and P. L. Kirk, Anal. Chem., 35 , 356 (1963).
022S. J. Mule, Anal Chem., 36 , 1907 (1964).